Balanitis xerotica obliterans (BXO) / lichen sclerosus of the male genitalia is a common cause of acquired phimosis, and was first described by Stuhmer in 1928 [1]. It is described in medical literature as a chronic inflammatory condition of unknown aetiology that affects the foreskin, glans and the external urethral meatus and urethra in severe cases.
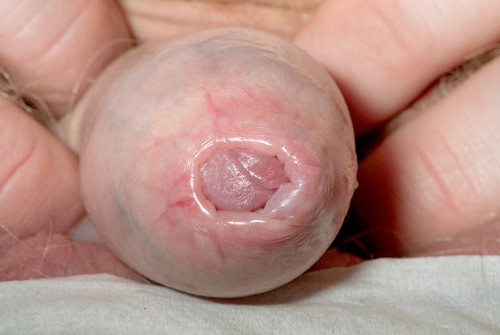
Figure 1.
Most patients present with phimosis with varying degrees of difficulty or inability to retract the foreskin [2]. The phimosis is usually progressive in nature with the presence of initially a white sclerotic ring in the distal prepuce (Figure 1) that becomes more apparent on retraction of the foreskin and at later stages complete inability to retract with fissuring and haemorrhagic blistering during sexual activity [2,3]. Obstructive symptoms, dysuria, poor urinary stream and urinary retention should also raise the suspicion of possible involvement of the external urethral meatus [2,4]. In aggressive cases, the surface of the glans and inner prepuce may ulcerate and fuse, therefore making circumcision technically difficult [3].
BXO can present at any decade with studies reporting an age range between two and ninety years. However, the highest incidence is reported in the third decade [5]. It is a common finding in urological practice, with the majority of cases being referred for consideration of circumcision due to the presence of phimosis.
Histological characteristics
Microscopically, marked fibrosis, epidermal atrophy, interface dermatitis, and dermal oedema are observed [6,7]. It is characterised by the presence of hyperkeratosis with an atrophic epidermis and with thinning of the rete pegs [6,7]. Dermal oedema with an increase in the number and size of the basal layer cells may also be present [6,7]. The papillary and reticular dermis present with a ‘washed out’ appearance with the dermal collagen forming a homogenous band at the dermal-epithelial junction in conjunction with elastin fibres, to produce an amorphous hybrid substance with infiltration of T lymphocytes, and less frequently B lymphocytes [6,7].
Aetiology
The aetiology of BXO is unknown. It demonstrates the Koebner phenomenon and arises from areas that have undergone trauma, old scars, skin graft and most importantly at sites prone to constant friction or after burns or radiation treatment [8].
Several studies have suggested that the warm, moist, urine-exposed environment that exists under the foreskin contributes to the pathogenesis of BXO. This explains why circumcision arrests the progression of the disease, whereas in cases where the circumcision was incomplete it can recur. Constituents in the urine leading to lichen sclerosus also explain why females present with vulvar lichen sclerosus as well as peristomal lichen sclerosus in patients with incontinent urinary diversion [3,9,10].
“Patients need to be educated with regards to BXO once diagnosis is confirmed and following circumcision, monitoring of the penile shaft skin and urethral meatus is required.”
Studies on lichen sclerosus of the female genitalia have also suggested an autoimmune association but the evidence is sparse in BXO [3,11]. There is no reported association between BXO and human papillomavirus infection, however other organisms and viruses such as acid-fast bacilli, spirochates, Borrelia burgdorferi and Epstein Barr virus have not been ruled out [12].
BXO and penile squamous cell carcinoma
Squamous cell carcinoma of the penis has been reported in patients with longstanding BXO. It is thought that the intermittent ulceration and chronic instability of the glans may contribute in the progression to penile squamous cell carcinoma [3]. The risk of malignant change in patients with BXO has been quantified in a few studies. Depasquale et al. reported a 2% rate in a cohort of 522 patients [3]. Nasca et at. calculated a 5.8% risk with a mean range of 17 years from diagnosis to malignant transformation. However, 80% of their cohort did have concomitant HPV infections [13]. In a retrospective study from the UK, Edmonds et al. reported a 0% risk following a review of 329 cases with BXO. All patients were diagnosed and treated effectively either with ultra-potent topical steroid or circumcision [14].
Management
The decision on whether to proceed or not with conservative or surgical treatment of BXO is dependent on the severity and the extent of the disease as well as the impact on the patient’s quality of life and patient’s choice.
Medical treatment
Topical steroids seem to offer a reliable option only in the management of mild BXO limited to the prepuce with minimal scar formation. Once established scarring and phimosis are present, steroids are ineffective [7]. In the early stages of this condition however, intermittent topical steroid therapy reduces disease progression and therefore the need for surgical management [15]. Recent evidence has additionally shown that intra-urethral steroids may also assist in the management of distal urethral strictures secondary to BXO [16].
Surgical treatment
Surgical management is reserved for cases with progressive phimosis or where conservative management has not been successful. The underlying benefit of performing a circumcision is to remove the urine exposed warm, moist environment provided by the foreskin aiding the development of BXO.
Circumcision is recommended when BXO is restricted to the foreskin with or without the involvement of the external urethral meatus.
In the presence of a urethral stricture, surgical procedures vary depending on the location of the stricture, the length and previous treatments. Therefore, urethral dilatation, urethrotomy and urethroplasty are all recognised treatments for the management of this disease [17,18].
Follow-up
Long-term monitoring of the foreskin is required in patients managed conservatively as progressive phimosis and adhesions between the inner prepuce and the glans may lead to a less favourable cosmetic result following circumcision. Recurrence of BXO is a recognised complication especially in individuals where the circumcision was incomplete or where there is a formation of ‘neo’-foreskin due to weight gain, increased pre-pubic fat and burying of the penis. Patients need to be educated with regards to BXO once diagnosis is confirmed and following circumcision, monitoring of the penile shaft skin and urethral meatus is required [19].
Good cosmetic and functional outcomes are dependent on the severity and the extent of the disease. Early diagnosis in primary care will enable timely conservative management under specialist dermatologist teams [20].
References
1. Stühmer A. Balanitis xerotic obliterans (post-operationem) und ihre Beziehungen zur “Kraurosis glandis et praeputii penis”. Arch F Dermat u Syph 1928;156:613.
2. Rickwood AM, Hemalatha V, Batcup G, et al. Phimosis in boys. Br J Urol 1980;52(2):147-50.
3. Depasquale I, Park AJ, Bracka A. The treatment of balanitis xerotica obliterans. BJU Int 2000;86(4):459-65.
4. Bale PM, Lochhead A, Martin HC, Gollow I. Balanitis xerotica obliterans in children. Pediatr Pathol 1987;7:617‑27.
5. Kizer WS, Prairie T, Morey AF. Balanitis xerotica obliterans: epidemiologic distribution in an equal access health care system. South Med J 2003;96(1):9-11.
6. Mihara Y, Mihara M, Hagari Y, Shimao S. Lichen sclerosus et atrophicus. A histological, immunohistochemical and electron microscopic study. Arch Dermatol Res 1994;286(8):434-42.
7. Hinchliffe SA, Ciftci AO, Khine MM, et al. Composition of the inflammatory infiltrate in pediatric penile lichen sclerosus et atrophicus (balanitis xerotica obliterans): a prospective, comparative immunophenotyping study. Pediatric Pathology 1994;14(2):223-33.
8. Bunker CB, Shim TN. Male Genital Lichen Sclerosus. Indian Journal of Dermatology 2015;60(2):111-17.
9. Ho BC, Cerio R, Bewley A. Lichen sclerosus associated with urinary contamina-tion. Eur J Dermatol 2016;26(1):109-10.
10. Al-Niaimi F, Lyon C. Peristomal lichen sclerosus: the role of occlusion and urine exposure? Br J Dermatol 2012;168(3):643-6.
11. Kreuter A, Kryvosheyeva Y, Terras S, et al. Association of autoimmune diseases with lichen sclerosus in 532 male and female patients. Acta Derm Venereol 2013;93:238-41.
12. Lau PW, Cook N, Andrews H, et al. Detection of human papillomavirus types in balanitis xerotica obliterans and other penile conditions. Genitourin Med 1995;71(4):228‑30.
13. Nasca MR. Innocenzi D, Micali G. Penile cancer among patients with genital lichen sclerosus. Journal of the American Academy of Dermatology 1999;41(6):911-4.
14. Edmonds EVJ, Hunt S, Hawkins D, et al. Clinical parameters in male genital li-chen sclerosus: a case series of 329 patients. J Eur Acad Dermatol Venereol 2012;26(6):730-7.
15. Folaranmi SE, Corbett HJ, Losty PD. Does application of topical steroids for lichen sclerosus (balanitis xerotica obliterans) affect the rate of circumcision? A systematic review. J Pediatr Surg 2018 [Epub ahead of print].
16. Potts BA, Belsante MJ, Peterson AC. Intraurethral steroids are a safe and effective treatment for stricture disease in patients with biopsy proven lichen sclerosus. J Urol 2016;195(6):1790-6.
17. Dubey D, Sehgal A, Srivastava A. Buccal mucosal urethroplasty for balanitis xerotica obliterans related urethral strictures: the outcome of 1 and 2-stage techniques. J Urol 2005;173(2):463-6.
18. Simsek A, Onol SY, Kurt O. Treatment of urethral strictures in balanitis xerotica obliterans (BXO) using circular buccal mucosal meatoplasy: experience of 15 cases. Arch Ital Di Urol 2014;86(1):23-5.
19. Homer L, Buchanan KJ, Nasr B, et al. Meatal stenosis in boys following circumcision for lichen sclerosus (balanitis xerotica obliterans). J Urol 2014;192(6):1784-8.
20. Boksh K, Patwardhan N. Balanitis xerotica obliterans: has its diagnostic accuracy improved with time? JRSM Open 2017;8(6):2054270417692731.
TAKE HOME MESSAGE
-
BXO is a common cause of acquired phimosis that affects the foreskin, glans and the external urethral meatus and urethra in severe and neglected cases.
-
It is suspected that the warm, moist, urine-exposed environment that exists under the foreskin contributes to the pathogenesis of BXO. This also explains why females present with vulvar lichen sclerosus as well as peristomal lichen sclerosus in patients with incontinent urinary diversion
-
Early diagnosis in primary care will enable timely conservative management under specialist dermatologist teams with better cosmetic and functional outcomes.
Acknowledgement: Figure 1 was used for this article following patient consent and retrieved from the Rotherham NHS Foundation Trust archive.
Declaration of competing interests: None declared.




