The COVID-19 pandemic has altered every aspect of how we live, and how healthcare needs to be provided for the welfare of patients and staff. I thought I would try to summarise a few potential technology tools that could be used by healthcare teams.
Microsoft Teams
Microsoft has provided NHS Digital and all NHSmail users with free access to Microsoft Teams [1]. Microsoft Teams is either browser based or downloadable onto a computer or mobile (Windows, MacOS, Android, iOS). The app facilitates one to one or multi-person video / audio conferencing in a secure environment. We trialled it within a cancer MDT environment, and I think it can work well but needs the MDT co-ordinator screen to be live shared, along with imaging / histopathology and the audio from the chair of the MDT. The rest of the MDT are probably better turning off their video and audio input, unless directly speaking, to save on bandwidth and reduce noisiness within patient discussions. In its current format, it is definitely not as good as being in the same room, but I think there could be working advantages to this type of format in the future.
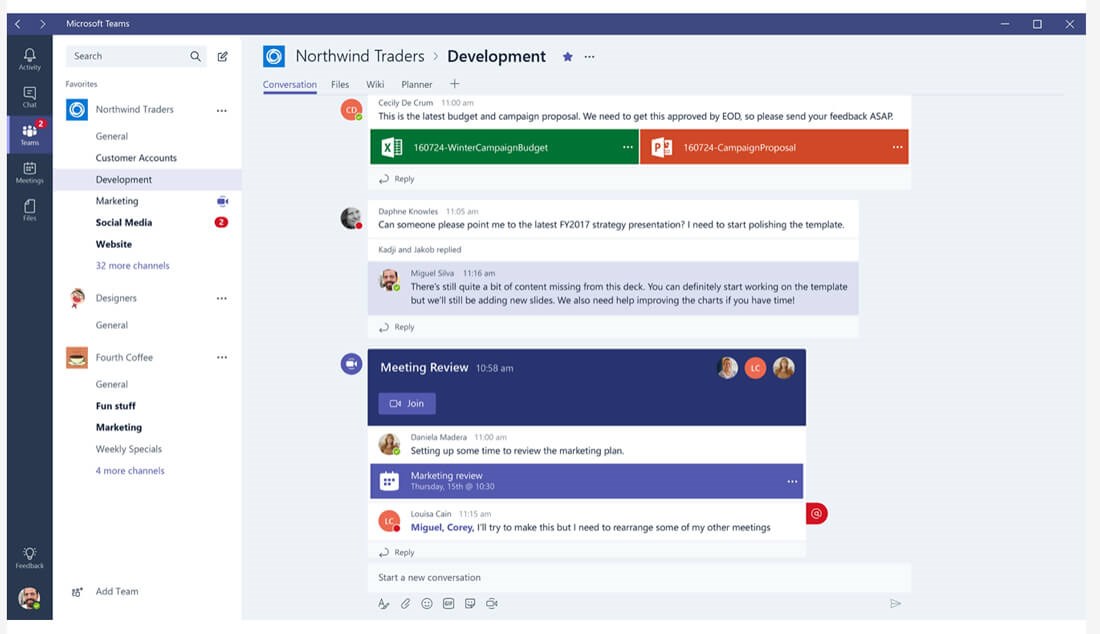
Microsoft Teams (image courtesy of Microsoft).
Slack
Slack is a browser-based alternative to email and direct messaging apps [2]. It allows key documents to be stored and shared with a team in folders which are called channels. Team members are invited by email and can then access the browser-based platform. There are mobile versions of slack for Android and iOS. Slack also allows one to one video conferencing between team members, and multi-person video / audio in the paid version. The free version allows up to 10,000 messages. Slack also integrates with Office 365 apps, Google apps and up to 2000 more which is great for team collaboration on projects.
The great advantage of Slack compared to email or messaging is that conversations are stored in a more organised manner. This is akin to using folders with email but in a more collaborative manner. It also means that long threads of email are not required as they are already grouped under a collective banner (channel). Any larger separate projects can have their own workspace created which can be accessed through your own web address (slack stores these automatically for all users). Slack’s servers are not entirely based in the European Union or UK and so patient details should be avoided at present. Currently, I see this as a potential platform for co-ordinating staff activity and discussion of various issues remotely, or co-ordination of a new service with all the problems that inevitably brings.
Siilo
Siilo is a messaging app [3] which is designed to replace messaging apps in a clinical environment. It is available for free on Android and iOS, and there is a web version that can be accessed with a QR code from your phone. The layout is very simple and slick with either Chats, Spaces or Settings options.
Chats has essentially the same layout as the popular messaging app, WhatsApp. Chats can be group discussions or individual messaging. Additionally, within the Chat group you can create a case and share information including photos and files. You could use case sharing for sharing potential cases with your immediate team or extended team of radiologists, pathologists, or for teaching proposes. Cases can be uploaded from the app into a patient’s electronic health record.
Spaces contains suggestions on people you may know (in the medical directory) and a list of all of the healthcare professionals registered within the NHS has been created during the COVID-19 emergency. Tapping on the ‘+’ in the bottom right corner allows users to create a group or chat, take a secure picture with your camera phone, scan a QR code or connect with colleagues. I have not used this yet for directly taking care of patients, but do believe that we should be using it widely within the NHS and there will be even more benefits and networks that can be developed if there is wide adoption of the app.
Attend Anywhere
Attend Anywhere [4], already in use in NHS Scotland, is a web-based platform that offers basic video call functionality for health and care providers. The platform has been made available throughout the UK and generates a weblink that providers can send to patients, which then activates a video call with patients at a set time. I have not yet had experience of this system. However, the key with implementing these services is ensuring that patients are able to use the services and are not excluded by the technology. There are also limited numbers of webcam-enabled PCs at most hospitals across the UK but I suspect most doctors have a webcam on their own personal laptop, as do most patients, so there should be scope to implement the technology quickly and securely.
BAUS
The British Association of Urological Surgeons has provided guidelines of the priority of cases that should be covered [5]. The guidelines are available through the members section of the website. Guidelines are currently available for prioritising surgery by type as well as condition e.g. bladder cancer, renal cancer, prostate cancer, penile cancer, testicular cancer and endourology. Obviously, this is a situation that is changing on a daily basis based upon local, regional and national resources. However, I think the broadness and speed of the guidance should be commended, particularly given that urology serves a primarily ‘at risk’ population for mortality from coronavirus.
EAU
The European Association of Urology has also created a page related to COVID-19 [6]. The page is not as comprehensive as the BAUS website’s information and does not cover everyday scenarios. It does put together some good links from the World Health Organisation as well as recent accepted papers in European Urology relating to COVID-19.
I hope this has covered a few bases which you might read about over the coming weeks or are already using. What are your technology suggestions for remote working in healthcare? What are your tips for making it work within the NHS? Tweet with the hashtag #covidtech or tag me @urolsurg in your tweet.
Links below or search for apps in the app stores
1. https://products.office.com/en-gb/microsoft-teams/group-chat-software
2. https://Slack.com
3. https://www.siilo.com/
4. https://www.attendanywhere.com/
5. https://www.baus.org.uk/about/coronavirus_covid-19.aspx
6. https://uroweb.org/covid19-resources-for-urologists/
All resources accessed 27 March 2020.





