Robotic fellowship training in the UK – overview
Robotic surgery has increased in popularity since its introduction in 2003. Its validation in a growing number of operative procedures has increased its acceptance nationwide and its usage is becoming widespread. Initial training of robotic surgeons relied heavily on industry and it is this training, which has helped to guide the first wave of robotic urological surgeons through their initial learning curve. The rapid introduction of robotic surgery throughout urology necessitates the introduction of standardised training methods.
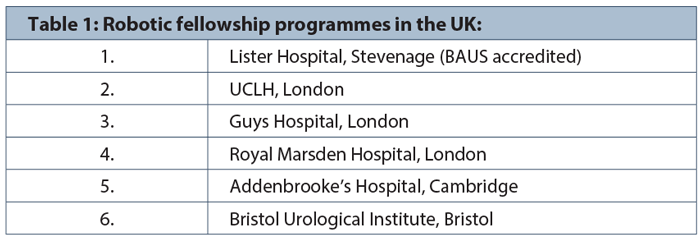
In the UK there are six fellowship programmes (Table 1) that give exposure to robotic fellowship training with the Lister Hospital being accredited by the Royal College of Surgeons of England and the British Association of Urological Surgeons (BAUS).These are extremely competitive, receiving applications internationally as well as from within the UK. Interest in these centres also comes from established urological consultants who are wishing to extend their practice to incorporate robotic surgery.
Robotic fellowships have the advantage of being based in well-established teaching hospitals with high volumes of robotic cases and robotic experience. Experience in a high-volume centre has been associated with the subsequent formation of a safe robotic unit in terms of functional and oncological outcome.
Despite the positive impact on individual training for robotic fellowships its introduction can be contentious. There is a risk that the presence of robotic fellows can impact negatively upon the training for established urology specialist registrars (SpR). Therefore, there has to be careful consideration regarding the division of labour and the provisions of training for all urology trainees. The role of the urology SPR can also be threatened by the introduction of advanced surgical nurse practitioners as bedside assistants in robotic surgery. Their introduction has added stability to the assistant role which may otherwise be a periodically rotating post with an adjustment phase required for each transition. Their relative wealth of experience may result in many urology trainees being outperformed when first learning to assist in robotics and therefore nursing assistants may become the favoured choice by many consultants.
There are several financial considerations when undertaking a career in robotic surgery. Courses are expensive and yet necessary for progression although a number of small grants and bursaries are available for support.
The Lister Robotic Fellowship
During my final year of training (ST7) in the Northern Deanery, Newcastle upon Tyne, I was very keen to pursue a structured fellowship in robotic urology prior to commencing my consultant post. I was very fortunate to be selected as the Robotic Urological Fellow at the Lister Hospital, Stevenage during the final six months of my ST7 training year.
My fellowship commenced in September 2012 on obtaining my CCT in urology and joining the specialist register in urology at the General Medical Council. Having had training in open / laparoscopic surgery during my specialist registrar rotation and assisted in 10 robotic prostatectomies I was fairly new to robotic surgery.
Figure 1. Initial Console training (Mr Jim Adhsead, Fellowship Director; Mr Nikhil Vasdev, RCSEng/BAUS Robotic Fellow; Dr Gowrie Mohan-S, Consultant Anaesthetist; Sister June Thomas, Charge Nurse Robotic Theatre).
Within a week of joining the fellowship and having a detailed induction with my fellowship supervisors I received a timetable which included time for operating (seven sessions a week), research (one session a week) and dry lab training (one session a week). The first three months were spent assisting in robotic urological procedures and learning docking / undocking of the robot and, more importantly, practising of emergency, steps for example rapid safe undocking in the event of a patient-related emergency such as an on-table cardiac arrest. I also learnt the importance of patient positioning and the prevention of clinical issues such as compartment syndrome and neurovascular injuries in relationship to the steep Trendelenburg position during robotic pelvic surgery. I spent my evenings and weekends coming to theatre and learning console control with the support of the theatre staff who, despite not being on call, would come in to set up the robot for me to practise suturing.
After three months, I was allowed onto the console in a stepwise manner practising initial steps of dissection followed by more advanced operative steps such as bladder neck preservation and different degrees of nerve sparing during robotic prostatectomy. The next six months were spent performing hilar dissection in robotic partial nephrectomy and completing the second layer renorraphy post clamp removal and completing robotic prostatectomies. By the end of nine months I had assisted and spent regulated time on the console in 140 cases.
The last nine months of my fellowship were spent becoming independent in robotic prostatectomy and robotic pyeloplasty. I also performed a majority of robotic cystectomies and intra-corporeal ileal conduit and neo-bladder formation. As my confidence grew I performed extended pelvic lymph node dissection. In total I was exposed to a further 160 cases in the last nine months of my fellowship where I was the lead console surgeon. Every case was video-recorded with patient consent and I spent time every evening watching these videos. I was never pressured by the anaesthetic team or the theatre team on time constraints although on certain days in the beginning theatre could over-run by up to two hours.
Figure 2. Our new dual console Si System.
During my fellowship we also obtained a dual console da Vinci® Si system , which has been of great advantage to training with the in-built simulator system. In addition to robotic urological surgery the fellowship was also very beneficial in improving my open / laparoscopic and endourological skills. I performed an additional 45 open cystectomies, 40 laparoscopic nephrectomies and 75 flexible ureterorenoscopies.
I met my supervisors every three months for a progress meeting and was required to submit a report to the Royal College of Surgeons of England at six-monthly intervals. During my meetings I viewed videos of my progress and received very useful feedback.
At the end of my fellowship I was awarded The Urology Foundation clinical visit grant to visit the Department of Robotic Urology at the City of Hope National Medical Center, Los Angeles, with Dr Timothy Wilson and Dr Clayton Lau. During my visit I learnt newer techniques in robotic retroperitoneal lymph node dissection and on-table robotic florescence techniques (Firefly™) technology for single kidney and complex robotic partial nephrectomy.
As the robotic fellow I published 23 papers, obtained three successful research grants, presented 35 abstracts at regional, national and international meetings and completed nine audits. I also completed a higher degree in urology (ChM (Urol)) at the University of Edinburgh and Royal College of Surgeons of Edinburgh under the supervision of Mr Jim Adshead with my thesis titled ‘Intraoperative frozen section of the prostate to reduce the risk of positive margin whilst ensuring nerve sparing in patients with intermediate and high-risk prostate cancer during robotic radical prostatectomy’. I obtained a distinction with my degree.
On the completion of my fellowship I was appointed as a Consultant Urological Surgeon at the Lister Hospital (East and North Herts NHS Trust) and Watford General Hospital (West Herts NHS Trust) in August 2014 and am performing robotic pelvic (prostatectomy / cystectomy / extended pelvic lymph node dissections / intra-corporeal ileal conduit formation / intraoperative frozen section of prostate) and robotic upper tract (robotic pyeloplasty / robotic nephrectomy / robotic nephro-ureterectomy). I am a Visiting Clinical Senior Lecturer in the Faculty of Medicine and Health Sciences at the University of Hertfordshire where we are developing a robotic haptic feedback programme and an enhanced recovery programme evaluation of intraoperative gut ischaemia during robotic surgery using intraoperative cytokine analysis. I am also a Clinical Tutor on the ChM (Urol) programme in robotic urology and new technology module at the University of Edinburgh and Royal College of Surgeons of Edinburgh.
In conclusion, the Lister Robotic Urological Fellowship is a great training opportunity in the UK for trainees to be exposed to and learn robotic urological surgery in a modular manner. It is an honour to become the first UK accredited robotic urology fellow by the Royal College of Surgeons and BAUS. Based on my experience as the RCSEng / BAUS Robotic Urological Fellow and now as a Consultant Urological and Robotic Surgeon training our next fellow, I can confirm that by using a regulated modular training methodology patient safety and outcomes are not affected [1,2]. We also welcome applications from highly motived trainees to apply for our fellowship programme.
References
1. Vasdev N, Bishop C, Kass-Iillya, et al. Developing a robotic prostatectomy service and a robotic fellowship programme - Defining the learning curve. Current Urology 2013;7:136-44.
2. Chan KE, Vasdev N. Current status of robotic training in the UK – a trainee’s perspective. International Journal of Cancer Therapy and Oncology 2014;2(1):02013.
Acknowledgment and thanks to:
Mr Jim Adshead, Mr Tim Lane, Mr Greg Boustead (Consultant Urological Surgeons, Lister Hospital). Dr Gowrie Mohan-S, Dr Venkat Prasad, Dr Raj Muralee (Consultant Anaesthetists, Lister Hospital). Ms June Thomas, Mr Jherico Ocampo, Mr Les Jones (Robotic Theatre Team, Lister Hospital). Dr Tim Wilson, Dr Clayton Lau (Consultant Urologists, City of Hope National Medical Centre, LA, USA). Ms Sarah Brooks (Urology Service Co-Ordinator). The Urology Foundation, UK.
Declaration of competing interests: None declared.





