As leading men’s health charity, Prostate Cancer UK, celebrates its 25th anniversary, top researchers reflect on the huge progress in testing, treatment and support for men over the past 25 years.
25 years of beating prostate cancer together
Matthew Hobbs, Director of Research, Prostate Cancer UK.
 A man diagnosed with prostate cancer in 1996, when Prostate Cancer UK was founded, faced a very different world than what we know today.
A man diagnosed with prostate cancer in 1996, when Prostate Cancer UK was founded, faced a very different world than what we know today.
Back then public awareness and medical understanding of the disease was basic. Treatment options were extremely limited, and damaging to quality of life, support outside of hospital was lacking, and, with very little money going into prostate cancer research, there was little hope of things changing. There weren’t any other prostate cancer-specific charities, and the government was investing little.
In the last 25 years we’ve boosted funding for prostate cancer research dramatically. Firstly, thanks to our supporters we’ve made a lot of noise to push prostate cancer up the agenda. Secondly, our funding has allowed researchers to build the evidence they need to get big grants from government, industry and other funders. Now the government is investing over £15 million a year. And since 1996, we’ve invested over £77.4 million into prostate cancer research, delivering huge benefits to men across the world. If this support continues, even bigger benefits are in sight.
To really make progress in scientific research you need far more than a single person, working on a single idea. You need a critical mass of researchers. Sometimes it’s about competition, having others working on similar things can push researchers to go faster. But mostly it’s about collaboration and conversation, sharing ideas and building on them to make the discoveries that accelerate progress.
That’s why one of the most important things we’ve done together is build a community of researchers dedicating their working lives to prostate cancer research. In 1996, there were no more than a handful of groups focused on prostate cancer. Now there are over 150 across the UK.
We’ve come a long way together, making many improvements in diagnosis and treatment for men with different stages of prostate cancer. We’ve punched above our weight because we have the best team in our corner. And that includes all the passionate and dedicated people who have supported us and worked with us in that time. Because of this hard work, thousands more men are living longer and experiencing fewer side-effects.
But we have a very long way to go. Too many men are dying and hundreds of thousands more experience side-effects that limit their lives.
Below, we meet some of the researchers dedicating their careers to prostate cancer. They reflect on some highlights in 25 years of progress for men across three key areas: diagnosis, localised disease and advanced prostate cancer. And share their plans for the future.
The long road to a screening programme
Prof Caroline Moore, Professor of Urology, University College London, UK.
Caroline Moore was the first female Professor of Urology in the UK. Her team at University College London specialises in developing MRI scans to improve diagnosis. She’s an expert in focal treatment and active surveillance. Here, Caroline shares her thoughts about how imaging has improved diagnosis in the last 25 years, and what she hopes to see in the future.
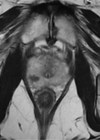
 Multi-parametric magnetic resonance imaging (mpMRI) has really allowed us to properly characterise men in a way we couldn’t before – even when we said men had no cancer after a negative biopsy we were wrong 50% of the time. Whereas now it’s maybe 3-4% of the time.
Multi-parametric magnetic resonance imaging (mpMRI) has really allowed us to properly characterise men in a way we couldn’t before – even when we said men had no cancer after a negative biopsy we were wrong 50% of the time. Whereas now it’s maybe 3-4% of the time.
Now a third of men can avoid a biopsy altogether and be reassured. And for men who do have a biopsy, we can be much more confident that we've found any disease that's there because we can use the scan to target areas of concern, instead of only random samples.
We used to say to men, you've got low-risk cancer, but there's a one in three chance that's high-risk, so maybe you should have surgery. That can be a distressing choice to make. Men still have very difficult choices, but now we can let men know if their cancer is low, intermediate or high-risk, which means they’ve a more accurate picture of the chances of progression, recurrence and side-effects and get to make a more informed choice.
Looking to the future, the big thing is whether we can develop a screening programme that will be both effective and cost-effective. We don't currently have one at the moment because the tools used in the last screening study - the combination of PSA and a standard biopsy - weren't good enough. I think as we refine our diagnostic tools, we can try again.
I hope we'll be able to set up a big screening study where we use modern diagnostic methods. That might include MRI, potentially more blood-based biomarkers, and risk calculators.
If we could have a screening programme, I hope we’d reduce the numbers of men diagnosed with metastatic disease that can’t be cured - currently between 14 and 16% of men. If we could find those men earlier through screening then we'd save many lives, and we'd save a lot of pain and suffering.
From one-size-fits-all to precision and personalisation
Prof Ananya Choudhury, Chair and Honorary Consultant in Clinical Oncology, The Christie NHS Foundation Trust, Manchester, UK.
Professor Ananya Choudhury leads a research group focused on personalised radiotherapy and localised prostate cancer. Her current project, funded by Prostate Cancer UK, is looking at tissue biomarkers to try and identify men with prostate cancer who have a poor prognosis and might benefit from additional treatments. Here Professor Choudhury reflects on the last 25 years of progress in treating localised prostate cancer.
 The information and knowledge out there now is much greater than it was 25 years ago. And as our medical technology has advanced, patient awareness has advanced too; with organisations like Prostate Cancer UK getting the message out, we now have more men being diagnosed with localised prostate cancer, when it’s still curable.
The information and knowledge out there now is much greater than it was 25 years ago. And as our medical technology has advanced, patient awareness has advanced too; with organisations like Prostate Cancer UK getting the message out, we now have more men being diagnosed with localised prostate cancer, when it’s still curable.
In 25 years we've also gone from very, very basic radiotherapy techniques through a number of technological advances. We used to treat large volumes of tissue either causing a lot of side-effects or using lower doses than we’d ideally need because for a lot of cancers, the higher dose you can give, the more you can cure.
We can be far more precise in locating the prostate and targeting only the area that needs treating. That’s enabled us to increase the dose and cure more cancers without increasing the side-effects. In some cases, we can now increase the dose and decrease the side-effects, which is like the Holy Grail. The evolution of brachytherapy also means, for men who are suitable, we can give very high doses of radiotherapy in a very concentrated form directly into the prostate. That was only just coming into play 25 years ago.
Men are also much more involved in the management of their prostate cancer and the decision-making process than they were 25 years ago. In medicine generally there’s been a switch from a paternalistic relationship between doctor and patient to a more collaborative one. We now have much more honest and transparent discussion with our patients about the pros and cons of what could be done for their prostate cancer. That has empowered men and I think it’s progress. But it does sometimes come at a cost.
All of us who work with these patients every day know there's a huge mental impact, not just of being told that you have cancer, but of feeling responsible for decision making as well. Many men have said to me, “But you're the doctor. You're the one who's meant to be an expert in this area, and now you're asking me to weigh up all this complex information and uncertainty and make a decision?”
What we really need is to be able to give men better information to make those decisions. A lot of men will never die of their prostate cancer and the decision is often around whether they're monitored or have an invasive treatment, but also around which treatment might be, not just best for the cancer, but best for them. At the moment we don't have the data and the ability to give detailed information about their own disease and the outcome. The more accurate our biomarkers and models are, the more we can empower men by giving them information to make that decision.
We might say to a man now, from what we know about your prostate cancer, we suspect it won't be a problem for decades and that you won't need treatment. But the difficulty for a lot of people is that the word cancer is so emotive. We use that one word to describe a whole spectrum of diseases. It's like infection, which can be anything from a tiny scratch on your toe that's gone a bit red to a life-threatening condition. Cancer can be very similar. Some cancers are life threatening, others you'd probably rather not know you had because the chances of them ever having an impact on you are very small.
We need more personalisation. For many of us in medicine, this dream almost feels like science fiction. But, given the uniqueness of each patient, what we'd like is a unique tailor-made management plan for that man. It would be lovely to be able to give our patients detailed information about the impact of their cancer over their lifetime. It might not be within 5-10 years, but I'd like to think within my lifetime.
Treating advanced prostate cancer: ‘A golden age of research’
Prof Johann De Bono, Consultant Medical Oncologist, The Royal Marsden NHS Foundation Trust, London, UK.
Professor Johann de Bono has led pivotal phase III trials of several prostate cancer drugs including, abiraterone, cabazitaxel, olaparib, enzalutamide and most recently the targeting of prostate-specific membrane antigen (PSMA) with radioactive lutetium. Johann has received over £10 million in grants since 2008 and is a major contributor to the research community.
 In 1996, a lot of men were diagnosed with advanced disease, meaning their prostate cancer had spread to other parts of their body and could no longer be cured. A man might have had hormone therapy, which was beginning to be available although it wasn’t well understood or widely used. Hormone therapy works by giving men drugs that starve prostate cancer of the male hormones that help it grow. Before it was available men would be treated with surgical castration to dramatically reduce their testosterone. Some men were still being treated that way in the mid-90s.
In 1996, a lot of men were diagnosed with advanced disease, meaning their prostate cancer had spread to other parts of their body and could no longer be cured. A man might have had hormone therapy, which was beginning to be available although it wasn’t well understood or widely used. Hormone therapy works by giving men drugs that starve prostate cancer of the male hormones that help it grow. Before it was available men would be treated with surgical castration to dramatically reduce their testosterone. Some men were still being treated that way in the mid-90s.
The biggest change in treatment for advanced prostate cancer in the last 25 years is the availability of new treatments. From the early 2000s until recently, the only option when hormone therapy stopped working was chemotherapy. Now we have new drugs like abiraterone, which our work helped to develop, and enzalutamide that can be given after traditional hormone therapy stops working. That means more men are surviving longer and having a better quality of life. We’ve also begun to see evidence that men can live longer if we give these drugs, in combination with docetaxel chemotherapy, much earlier on in their treatment journey.
We now have a much better understanding of the biology of prostate cancer than we had even 10 years ago. We understand the complexity – it’s not just one disease which we can treat uniformly, but many different diseases that need different approaches.
This has opened up totally new ways to treat advanced disease. We’re becoming much more precise and getting closer to being able to give the right treatment, for the right man, at the right time so men can avoid wasting extremely precious time on treatments that are unlikely to work. We’re now starting to see clinical trial results showing that we can use targeted treatments for specific prostate cancers and those will expand our arsenal of drugs even further.
We’ve worked to understand the internal mechanisms of the prostate cancer cell and have translated those into ways to kill tumour cells while sparing the patient’s normal cells.
We were the first to show that drugs called PARP inhibitors, like olaparib, work in some prostate cancers – DNA repair defective prostate cancers. I have men today in my clinic who would be dead if we hadn’t done that work. Those drugs will be the first therapies for advanced prostate cancer that are targeted down at a molecular level.
Now we need to keep working to find weaknesses in other prostate cancers so we can develop more targeted agents to attack them and benefit the greatest number of men.
The next challenge is figuring out who needs what treatment. We need to use what we’ve learned to develop treatment strategies that can target specific mutations in a man’s prostate cancer or things that are driving individual cancers to grow and spread.
In future I hope we’ll be able to do this much more precisely. And we’re starting to see that with drugs like PARP and AKT inhibitors such as olaparib and ipatasertib. But there’s a long way to go. I hope we’ll also work out how to prevent, or at least get ahead of, cancers developing resistance to effective treatments. And we need to train the next generation of research leaders to take all of this forward.
This is a golden age of prostate cancer research. The research we, and others, have done over the past 25 years means we now know a lot more about the opponent we’re facing. It’s also shown what a formidable opponent prostate cancer is. It is only by understanding the disease and all its complexity that we’ll make the huge improvements in survival and quality of life that men with advanced prostate cancer urgently need. We’re now in a position, armed with knowledge, to deliver that through research over the next 25 years.
For more information visit www.prostatecanceruk.org

Prostate Cancer UK is a registered charity in England and Wales (1005541) and in Scotland (SC039332).
Registered company 02653887.
See Also: Prostate Cancer Focus