COVID-19 had a major impact on our hospital services from early in the pandemic, with almost three times as many patients being ventilated compared to the normal ITU capacity at the beginning of April. During the build-up to this point, contingency plans had already been put in motion for the conversion and utilisation of main theatre space as ITU beds. This saw an end to all our elective operating by 27 March. Various surgical wards were merged to accommodate an anticipated higher demand from medical admissions.
All foundation year one doctors were re-deployed to medicine and the senior house officer grades within the surgical department were pooled into a mixed general surgery and ITU ‘COVID rota’. In the outpatient setting, clinics were converted to either telephone or remote video consultations, with face-to-face appointments reserved only for breaking bad news and suspected cancer referrals requiring examination.
This initial period held a lot of uncertainty, with plans to provide cancer services often being changed on an almost hourly basis. During these delays, our unit had already seen patients suffer stage progression whilst awaiting surgery, highlighting the desperate need to find a way to re-open some of our services. Flexible cystoscopy lists and haematuria clinics were moved to private facilities and performed by our department’s registrars. At the same site, two all day theatre lists per week were also arranged, dedicated to bladder tumour resections and urgent stone cases. Prostate biopsies were put on hold due to lack of facilities and safety concerns.
Pre-COVID, our unit had been performing transperineal prostate mapping with cognitive target biopsies routinely since May 2014. Like many other centres, this had been conducted under general anaesthetic in day case theatres. With the use of a transperineal access system, our department had begun to shift towards local anaesthetic transperineal prostate biopsy (TPPBx) since mid-2019. This was, however, within the familiar comfort of day stay theatres meaning the option of sedation was always available (and often used). After the pandemic hit we encountered frequent scheduling difficulties and completely lost day stay theatre capacity.
Particularly at the beginning of the crisis, there were concerns regarding the safety of the procedure to staff given the aerosol generating nature of transrectal ultrasound (TRUS). We were also not keen to return to transrectal biopsy due to complication risks such as urosepsis, which would not only put patients at excess risk but potentially strain the already stretched resources and hospital capacity limits. Amongst the disruption however, new facilities became apparent. The outpatient department and cystoscopy room were now almost empty and many of the outpatient staff were not required for re-deployment. We therefore utilised the space and personnel in order to start a true local anaesthetic TPPBx service within the outpatient setting.
Establishing a new service during the COVID-19 pandemic required careful planning and preparation. From mid-May arrangements began to take form. Patients awaiting biopsy were triaged into high and low-risk based on the prostate specific antigen (PSA) level and MRI Prostate Imaging Reporting and Data System (PIRADS) score. Low risk was categorised as PIRADS score <3 or PSA density <0.15ng/mL2, and patients scheduled for routine active surveillance biopsy (standard repeat biopsy at 12 to 24 months according to repeat PSA and MRI findings). This group was deferred or placed onto PSA surveillance which left 42 men awaiting biopsy (mean age 69 years, SD ±6). These men were all contacted and, following a telephone consult regarding COVID-19 risk, were offered a local anaesthetic TPPBx. Subsequently they attended a nurse led face-to-face pre-assessment approximately one week before biopsy.
During this appointment, they were counselled and consented for the procedure; had a urine sample and COVID-19 swab taken; received anti-coagulation or anti-platelet advice; supplied with prophylactic antibiotics (oral ciprofloxacin 500mg to be taken the evening before and the morning of the procedure) and antimicrobial body wash; and provided with isolation instructions. During full lockdown patients were asked to self-isolate for 14 days prior to their procedure, with easing of lockdown measures this has now reduced to seven days (at the time of writing). Any positive urine cultures were treated according to antimicrobial sensitivities, and the procedure was postponed until a negative sample was received. To minimise contact and potential infection spread, patients were given specific time slots to arrive and not permitted to have accompanying relatives or friends, thus avoiding multiple people in the waiting areas at any given point.
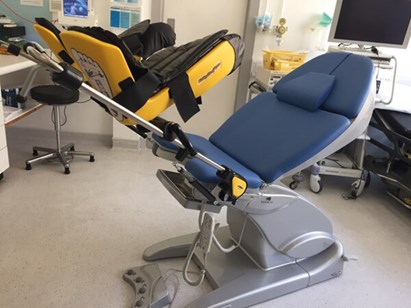
Figure 1.
Our outpatient flexible cystoscopy room was adapted with an examination couch (chair model: arco with side rails, SCHMITZ u. Söhne GmbH & Co. KG) and stirrups (Figure 1). The level of personal protective equipment (PPE) was developed in accordance with guidelines from Public Health England and further adapted for performing TPPBx. The operating surgeon and assistant both wear a sessional gown, gloves, FFP3 mask, and eye protection; alongside single use aprons and sterile gloves. The circulating nurse dons sessional eye protection and fluid resistant mask with disposable gloves and apron. The patient is provided with a surgical face mask if they have not brought their own face covering. Donning and doffing areas were adapted to space availability and undertaken within the procedure room.
Biopsy is performed under TRUS guidance in a dorsal lithotomy position. A digital rectal examination helps relax the anal sphincter. The perineal skin is cleaned with a chlorhexidine solution and ethyl chloride spray applied topically. Local anaesthetic (10mL lignocaine 1% with adrenaline) is then infiltrated to the perineal skin. Under TRUS guidance, 7.5ml of plain 1% lignocaine is then infiltrated to each side (15ml total) approximately midway between the midline and the lateral border of the prostate, as well as the needle tract from the apex of the prostate back to the skin. This also provides an opportunity to assess the depth and height of the gland in relation to the chosen level of access needle placement.
The TRUS probe is then removed for six minutes to allow the anaesthetic to diffuse. Both cognitive target and systematic samples are then taken via the perineal access needle, which is punctured bilaterally. In our department, we have used the PrecisionPoint™ transperineal access system (BXTAccelyon) (Figure 2) but other products are available, such as Trinity™ (KOELIS) and CamPROBE (University of Cambridge and Cambridge University Hospitals).

Figure 2.
The cancer detection for this cohort was 32/42 (76%) for any cancer and 26/42 (62%) for Gleason grade ≥4+3 and / or maximum cancer core length ≥6mm. These compared favourably to the predicted detection rates of 69% and 55% respectively; calculated by our previously internally validated nomogram based on age, PSA density, MRI PIRADS score and prior biopsy status [1]. The vast majority of patients tolerated the procedure very well and had targeted and systematic biopsies where indicated. Two were able to tolerate targeted biopsy cores but declined further sampling. There were no cases of infection or retention, and no patients developed clinical signs of COVID-19.
At a comfortable capacity of eight patients per day and a couple of lists per week, we cleared our backlog within a month. Three registrars in the department became competent in the technique very quickly; we have now started to train our nurses in the procedure to be able to deliver a nurse-led service in the future. Use of outpatient staff to support the procedure has led to continuity of care within the diagnostic pathway.
In our experience TPPBx under local anaesthetic has been safe, well-tolerated, and maintains diagnostic efficacy. It is practical in the outpatient setting and avoids the risks associated with general anaesthesia and transrectal prostate biopsy. The COVID-19 pandemic presented an unexpected opportunity to develop and improve our service.
References
1. Lee SM, Liyanage SH, Wulaningsih W, et al. Toward an MRI-based nomogram for the prediction of transperineal prostate biopsy outcome: A physician and patient decision tool. Urol Oncol 2017;35(11):664.e11-664.e18.
Declaration of competing interests: None declared.
Acknowledgments:
-
Prostate Cancer UK Leading Improvement Programme.
-
Mr Rick Popert (Guy’s and St Thomas’ NHS Foundation Trust) - mentorship of service.
-
Images provided by BXTAccelyon.






