Introduction
Erectile dysfunction (ED) is defined as the inability to achieve and maintain a penile erection, which is adequate for satisfactory sexual intercourse. The Massachusetts Male Ageing Study (MMAS) reported the results of a regional survey of men aged 40–69 years. In this study 52% reported some degree of ED with an increased risk as men get older.
Physiology of penile erection
Penile erection is a complex neurovascular event. The degree of contraction or relaxation of the smooth muscle within the corpus cavernosum will determine the level of penile tumescence. Contractile and relaxant factors are controlled by both central and peripheral mechanisms and involve the interaction of three different systems:
A. The central nervous system.
B. The peripheral nervous system.
C. Vascular and cavernosal smooth muscle in the penis.
The central nervous system
The central nervous system (CNS) co-ordinates incoming sensory information from a variety of sources, which may be visual, auditory, cognitive or imaginative, tactile or olfactory. The central pathways integrating these inputs and controlling erectile function are complex and still not completely understood. However, the paraventricular nucleus (PVN) and the medial pre-optic area (MPOA) within the hypothalamus control erectile function. The MPOA is thought to be an integrative centre that collects and redistributes signals to other areas within the CNS such as the PVN. The PVN in turn has been suggested to activate selective autonomic pathways leading to a penile erection. The neurons from the PVN project onto the spinal cord either directly or via the median forebrain bundle, pons and medulla and involve a number of neurotransmitters e.g. oxytocin, vasopressin, encephalin and dopamine.
The peripheral nervous system
The thoraco-lumbar erection centre is located between T1 and L2 and gives rise to the sympathetic outflow pathway. This connects to the urogenital tract via the pelvic, cavernosal and pudendal nerves. The sacral erection centre is located between the S2 and S4 segments of the spinal cord and gives rise to the parasympathetic outflow pathway. Nerve fibres reach the penis via the pelvic, cavernosal and pudendal nerves. Furthermore, the penis receives dense somatic input from sensory branches of the dorsal nerve, a branch of the pudendal nerve.
The individual nerves innervating the penis may contain a number of different neurotransmitters and as a result the nerves are categorised as either being adrenergic or cholinergic according to the predominant transmitter present. Nitric oxide (NO) is the neurotransmitter, which will mediate relaxation of the penile smooth muscle.
NO is released from parasympathetic nerve terminals (nitrergic nerves) via neuronal nitric oxide synthase (nNOS) and results in relaxation of the cavernosal smooth muscle and vasodilation. A further source of NO is derived from the vascular endothelium via endothelial nitric oxide synthase (eNOS) secondary to sheer stress. Noradrenaline released from sympathetic nerves results in vasoconstriction and an increase in the smooth muscle tone within the corpus cavernosum eventually leading to penile detumescence. A balance between pro- and anti-erectile mediators therefore regulates the erection of the penis.
Anatomy of the penis
The human penis is composed of paired corpora cavernosa and the single corpus spongiosum. The corpus cavernosum consists of a meshwork of sinusoidal spaces lined by endothelial cells. In order for an erection to occur, relaxation of corpus cavernosum smooth muscle allows blood to flow into the penis with an increase in the intra-cavernosal pressure. This is followed by compression of the subtunical venules against the tunica albuginea and a reduction of the venous outflow from the corpora cavernosa. With full tumescence the intracavernous pressure can be higher than systemic (systolic) blood pressure with the contribution of the skeletal muscles of the pelvic floor.
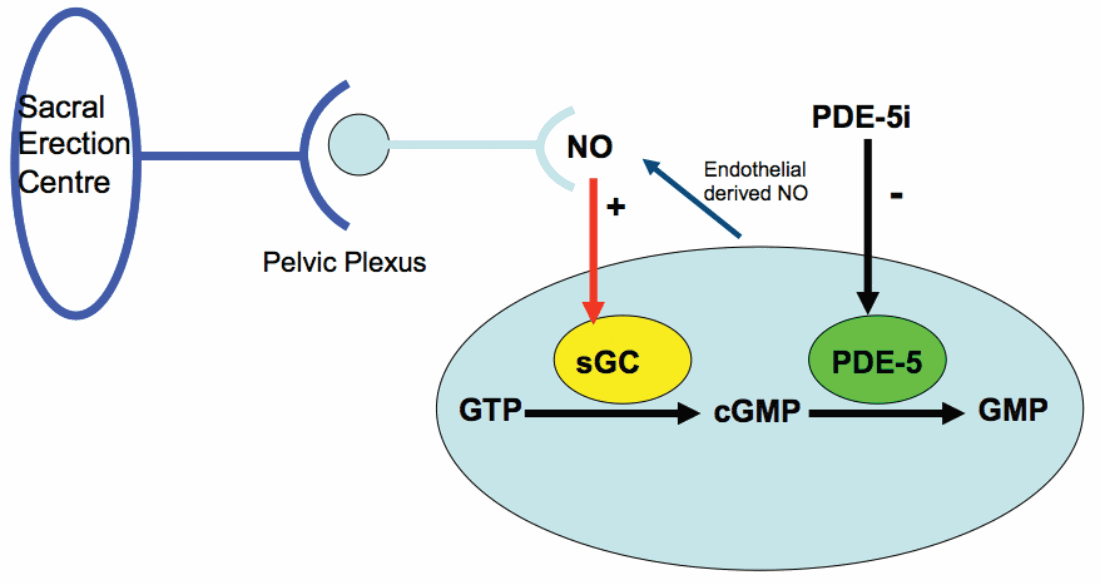
Figure 1: Nitric oxide (NO) released from nitrergic nerves and endothelium stimulates smooth muscle relaxation by activation of soluble guanylate cyclase (sGC), which in turn catalyses the conversion of GTP to the active intracellular second messenger cGMP. cGMP is then metabolised by PDE5 to inactive GMP.
The NO-sGC-cGMP pathway
Once released, NO exerts its action on smooth muscle cells by activating the enzyme soluble guanylate cyclase (sGC). The activation of sGC results in an increase in intracellular cGMP concentrations (Figure 1). This in turn activates a number of second messenger systems, which ultimately results in smooth relaxation. The cGMP is then metabolised by the enzyme phosphodiesterase type 5 (PDE-5).
Pathophysiology of erectile dysfunction
ED is commonly divided into either psychogenic or organic causes. However in many patients the disorder is of mixed aetiology with both factors contributing. The psychogenic component of ED is reported to be especially important in younger men (aged less than 35 years). Diseases, which become more prevalent with age such as diabetes and vascular disease, are major risk factors in the ageing male as well as major pelvic surgery e.g. radical prostatectomy. Concomitant drug treatment is also a risk factor with the commonly prescribed drug groups listed in Table 1.
Table 1.
Antidepressants
SSRIs / MAOIs / Tricyclic antidepressants
Antihypertensives
β blockers / Verapamil / Methyldopa / Clonidine / Reserpine / Guanethidine
Cardiac
Digoxin / Amiodarone
Diuretics
Spironolactone / Thiazide
Hormona
Antiandrogens (flutamide, cyproterone acetate) / LHRH agonists (leuprolide, goserelin) / 5 α reductase inhibitors / Corticosteroids / Ketoconazole
H2 antagonists
Cimetidine / Ranitidine
Recreational drugs
Alcohol / Marijuana / Cocaine
ED associated with diabetes and vascular disease is a result of endothelial dysfunction and neurogenic injury. With pelvic surgery, damage to the cavernosal nerves is the predominant cause. Other common risk factors include Peyronie’s disease, spinal cord injuries and neurological diseases. Since ED and coronary artery disease share a number of common risk factors, the commonality of endothelial dysfunction in both conditions has now been proposed. ED is considered another manifestation of vascular disease specific to small-vessels and an early manifestation of systemic endothelial dysfunction.
Moreover, endothelial dysfunction is a reflection of the loss of NO activity or biosynthesis at the endothelial level. This is associated with vasoconstriction, coagulation, leucocyte adhesion and smooth muscle cell hyperplasia, which is central to the process of atherosclerosis. The inhibition of eNOS (via impaired hydrolysis of dimethyl arginine) and the uncoupling of eNOS activity increases the oxidative stress in the endothelial cells. In diabetes associated endothelial dysfunction, elevated free fatty acids which are seen in patients with insulin resistance, may induce endothelial dysfunction through the activation of protein kinase C (PKC), the increased production of reactive oxygen species (ROS), elevation in triglyceride and LDL, and decrease in HDL levels.
More recent evidence suggests that the effects of hyperglycaemia and insulin resistance on endothelial cells are additive, since defects in both glucose and lipid metabolism produce similar effects with the resultant decrease in endothelial NO availability. The association between metabolic syndrome, insulin resistance and obesity and ED in men is now well characterised and understood. A number of epidemiologic studies have reported an increased risk of ED in diabetic men with a prevalence of between 35-50% in diabetic patients. In diabetes, the severity of ED has been demonstrated to be related to both the severity, and duration of diabetes. There is a higher incidence of peripheral neuropathy, autonomic neuropathy, microangiopathy and arterial insufficiency in diabetic patients with ED than in potent diabetic patients.
The proposed mechanisms of ED in diabetics include: elevated advanced glycation end-products (AGEs) and increased levels of oxygen free radicals, impaired nitric oxide (NO) synthesis, decreased and impaired cyclic guanosine monophosphate (cGMP)-dependent kinase-1 (PKG-1), increased endothelin B (ETB) receptor binding sites and ultrastructural changes, upregulated RhoA/Rho-kinase pathway, endothelial dysfunction and NO-dependent selective nitrergic nerve degeneration.
TAKE HOME MESSAGE
-
Erectile dysfunction is often a combination of organic and psychogenic causes.
-
Nitric oxide (NO) is the principal neurotransmitter.
-
Erectile dysfunction is a manifestation of endothelial dysfunction.
Part 2 of this topic is available here.