Epidemiology
Seminal vesicle calculi are uncommon with just over 100 cases being reported in the literature, although the true incidence is likely to be higher [1-9]. Patients usually present aged between 30 and 45 years old and although the pathogenesis of the stone formation is unclear, a high index of clinical suspicion and appropriate investigations can lead to the diagnosis [1].
Pathogenesis
Stone analysis provides composition information and possible pathogenesis. In most cases these stones are comprised of proteinaceous material but carbonate apatite, calcium oxalate and calcium fluorophosphate stones have also been reported [8-10]. The suggested pathogenesis for their formation includes: seminal vesiculitis, anatomical abnormalities of the seminal vesicle predisposing to stasis and urinary reflux into the ejaculatory ducts [1,5].
Clinical presentation
Most patients present with a history of passing stones or grit during ejaculation which is occasionally accompanied by pain and haematospermia [1,4]. Ejaculatory duct obstruction secondary to calculi can occur in patients with seminal vesicle stones and can result in infertility [3,5]. These stones are occasionally palpable during rectal examination and can be sometimes confused with tuberculosis calcification of the seminal vesicle and vas deferens [11].
Investigations
Semen analysis should be performed as bilateral obstructive calculi could be a cause for obstructive azoospermia [2,7]. Initial serum investigations include renal function tests, and calcium and uric acid levels to exclude predisposing conditions for stone formation.
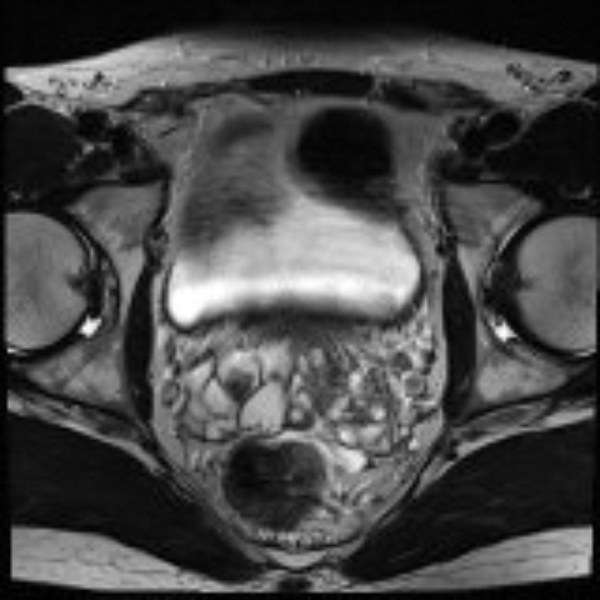
Figure 1: MRI image showing calculi in bilateral seminal vesicle.
Transrectal ultrasound (TRUS) is a safe non-invasive technique and is performed initially to view the prostate and seminal vesicles and can also diagnose seminal vesicle dilatation, calculi and seminal vesiculitis [1,6]. However, MRI (Figure 1) offers a 3D view of the seminal vesicles and allows surgical planning [6,10].
Occasionally, interventional imaging of the seminal vesicles is required to exclude anatomical abnormalities. One approach is with a vesiculoscope and retrograde imaging via catheterisation of the ejaculatory ducts. Another approach is antegrade imaging of the seminal vesicles after a TRUS guided injection of contrast referred to as seminal vesiculography (Figure 2).
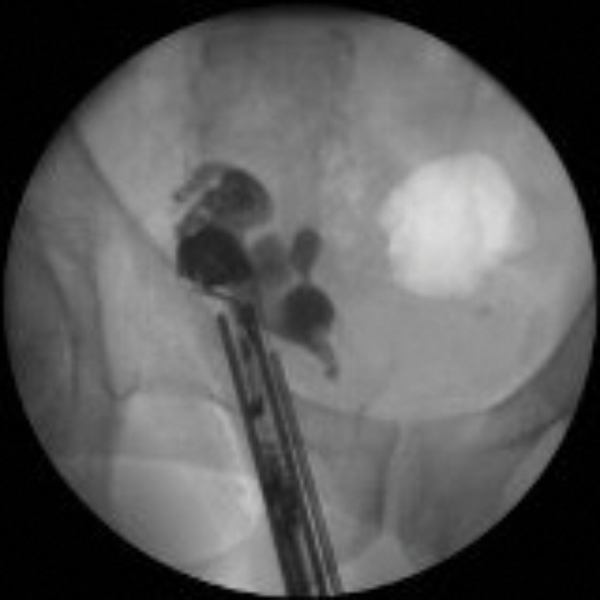
Figure 2: Antegrade seminal vesiculoscopy showing a stone close to the right ejaculatory duct.
Management
Seminal vesicle stones have been treated in the past by open vesiculectomy especially when these were multiple and large [3]. However, this procedure involves major pelvic surgery and can be a significantly morbid procedure due to the anatomical position of the seminal vesicles.
Minimally invasive techniques have developed since then and in cases of ejaculatory duct obstruction, transurethral resection of the ejaculatory duct (TURED) can be performed. This procedure has been associated with a higher risk of complications, including the impairment of semen parameters and retrograde ejaculation. TURED should only be performed in patients with confirmed obstruction and small volume calculi [2].
“Most patients present with a history of passing stones or grit during ejaculation which is occasionally accompanied by pain and haematospermia.”
Transurethral seminal vesiculoscopy (TRU-SVS) is a highly specialised technique and can be performed using a 6F endoscope. It has been used in some case series for the investigation of persistent haematospermia or ejaculatory duct obstruction but also to fragment and remove small seminal vesicle stones [1,2,3]. The use of LASER lithotripsy with a ureteroscope has also been recommended for seminal vesicle stones [9].
Laparoscopic or robot assisted vesiculectomy for larger stones is feasible via a transperitoneal approach [7,10]. It also allows anatomical correction of the seminal vesicle as these often remain dilated after stone extraction, or when the stone has formed in a seminal vesicle cyst [7,10]. This can be performed by pelvic surgeons with experience in minimally invasive pelvic surgery.
Conclusion
Treatment options for the management of seminal vesicle stones are still being developed and symptomatic patients should be offered treatment once the stones are diagnosed. Small case series in specialised centres report good stone clearance rates and symptomatic relief [1].
TAKE HOME MESSAGE
-
Patients reporting haematospermia or sperm containing calculi following ejaculation should be investigated appropriately to exclude ejaculatory duct or seminal vesicle stones.
-
Small seminal vesicle stones can be treated with transurethral seminal vesiculoscopy. When large and multiple, laparoscopic approach or robot assisted surgery can be considered.
References
1. Song T, Zhang X, Zhang L, et al. Transurethral seminal vesiculoscopy in the diagnosis and treatment of seminal vesicle stones. Chin Med J 2012;125(8):1475-8.
2. Wang H, Ye H, Xu C, et al. Transurethral seminal vesiculoscopy using a 6F vesiculoscope for ejaculatory duct obstruction: initial experience.
J Androl 2012;33(4):637-43.
3. Modi PR. Case Report: endoscopic management of seminal vesicle stones with cutaneous fistula.
J Endourol 2006;20(6):432-5.
4. Ozgok Y, Kilciler M, Aydur E, et al. Endoscopic seminal vesicle stone removal. J Urol 2005;65(3):591.
5. Kilciler M, Saglam M, Ozgok Y, et al. Giant seminal vesicle stones. Report of two cases. Urol Int 2002;69(3):250-1.
6. Namjoshi SP. Large bilateral star-shaped calculi in the seminal vesicles. J Postgrad Med 2002;48(2):
122-3.
7. Gordon Z, Monga M. Endoscopic extraction of an ejaculatory duct calculus to treat obstructive azoospermia. F J Endourol 2001;15(9):949-50.
8. Yun SJ, Kim T-H, Kwon W-A, et al. A large stone in the dilated left seminal vesicle: Laparoscopic Removal and Partial Seminal Vesiculectomy. Korean J Urol 2008;49:656-8.
9. Cuda SP, Brand TC, Thibault GP, Stack RS. Case report: Endoscopic laser lithotripsy of seminal-vesicle stones. J Endourol 2006;20(11):916-18.
10. Han P, Yang Y-R, Zhang X-Y, Wei Q. Laparoscopic treatment of a calcium fluorophosphates stone within a seminal vesicle cyst. Asian J Androl 2008;10(2):337-40.
11. Stasinou T, Bourdoumis A, Owegie P, et al. Calcification of the vas deferens and seminal vesicles: a review. Can J Urol 2015;22(1):7594-8.




