Case 1
A 67-year-old man presents with a worsening red patch over the past three months. It looks velvety in some areas.
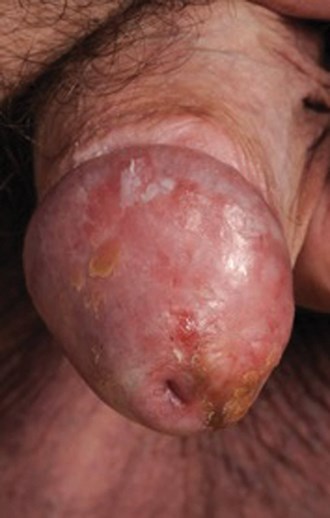
- What is the most likely diagnosis?
- What are the risk factors?
- How do you classify this condition?
- How are you going to confirm your diagnosis?
- Your diagnosis is confirmed. This is a superficial lesion. What are the treatment options?
Case 2
A 68-year-old man presents with a penile lesion. Biopsies have confirmed penile squamous cell carcinoma (SCC). MRI showed a tumour invading the spongiosus tissue of the glans. Lymph nodes were not palpable and not pathologically enlarged on MRI.
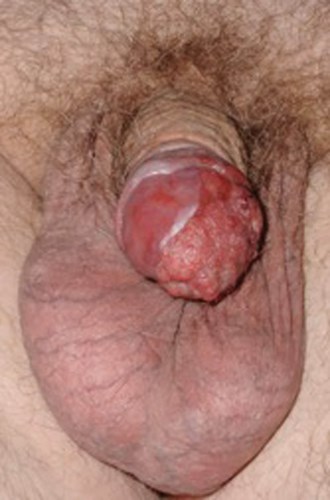
- What is the T stage?
- What are the common subtypes of penile carcinoma?
- Histology shows G3 T2 confined to the glans. What are his management options?
Case 3
A 69-year-old man presents with a penile mass. On palpation, this is confined to the distal penis and no inguinal lymph nodes were palpable. MRI shows a distal penile lesion invading the corpus cavernosum with no pathologically enlarged lymph nodes.
- What is the MRI T stage?
- His biopsy confirms G3 penile SCC. What is his surgical option and what are the complications of this procedure?
- A dynamic sentinel lymph node biopsy was performed. What radioactive tracer is used and what do you inject intraoperatively?
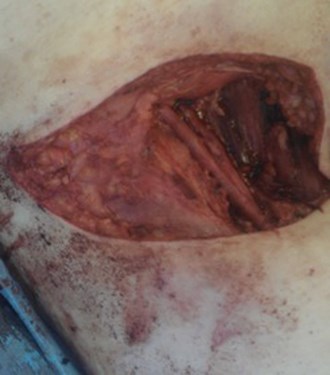
- His sentinel lymph nodes were positive for SCC on one side. What is being performed in the figure? What are the anatomical boundaries of this procedure? What are the complications?
Acknowledgement:
Figures are reproduced from Johnston MJ and Nigam R. Recent advances in the management of penile cancer [version 1; peer review: 2 approved]. F1000Research 2019, 8(F1000 Faculty Rev):558 (https://doi.org/10.12688/f1000research.18185.1).
Penile cancer: answers
Case 1
- Penile intraepithelial neoplasia (PeIN). Previous terms used include carcinoma in situ (Cis), Erythroplasia de Querat and Bowen’s disease. This is a pre-malignant condition for invasive penile squamous cell carcinoma (SCC) and may progress in approximately 10% of cases.
- Penile cancer is a rare condition, approximately 710 cases in the UK in 2017. The risk factors include phimosis, chronic penile inflammation (e.g. lichen sclerosis, balanoposthitis), smoking, HPV 16/18, Ultraviolet A or Psoralen treatment for psoriasis.
- Differentiated (lichen sclerosis associated) or un-differentiated PeIN (HPV associated). Warty, basaloid, warty-basaloid PeIN.
- Circumcision (if uncircumcised) and incisional biopsy of the lesion. 5. Topical agents with 5-fluorouracil (complete response rate approximately 57%) or imiquimod, laser with CO2 or Nd-YAG (recurrence 11-26%), glans resurfacing (local recurrence 4-6%).
Case 2
- cT2. Ta: non-invasive verrucous carcinoma; T1a: tumour invades subepithelial connective tissue without lymphovascular invasion (LVI) and is not poorly differentiated; T1b: invades subepithelial tissue with LVI or is poorly differentiated; T2: invades corpus spongiosum with or without urethral invasion; T3: invades corpus cavernosum with or without urethral invasion; T4: invades other adjacent structures.
- Squamous cell carcinoma (48-65%), basaloid carcinoma (4-10%, poor prognosis), warty (7-10%, good prognosis), verrucous (3-8%, good prognosis), papillary (5-15%, good prognosis), sarcomatoid (1-3%, very poor prognosis), warty-basaloid (9-14%, poor prognosis). Under 1%: pseudohyperplastic, carcinoma cuniculatum, pseudoglandular, adenosquamous, mucoepidermoid.
- European Association of Urology (EAU) guidelines: wide local excision, glansectomy +/- split skin graft, radiotherapy if tumour diameter is <4cm. Although his MRI showed no pathological lymph nodes, this will not detect micro-metastasis (up to 25%). EAU recommend further evaluation such as performing dynamic sentinel lymph node biopsy (DSLNB) for intermediate-risk lesions (G2 T1) and high-risk lesions (G3, ≥T2).
Case 3
- T3. The MRI is performed following intra-cavernosal injection with caverject.
- Partial penectomy if he has a penile stump of 5cm and wants to maintain function. Complications: infection, bleeding, meatal stenosis, spraying of urine, penile shortening, altered sensation, sexual dysfunction, disease recurrence. EAU recommend a surgical margin of 3-5mm.
- The first part (radiological) involves peri-tumour injection of Technetium 99-nanocolloid followed by static images. Lymph node location is marked by the radiologist. The second part (surgical) involves peri-tumour injection; approximately 1ml of patent blue. Inguinal incisions are made, and with the Geiger counter, the ‘blue’ node(s) with a high count is localised and excised.
- Inguinal lymph node dissection. Boundaries: superior, inguinal ligament; medial, lateral border of the adductor longus; lateral, medial border of the sartorius; Inferior, apex of the femoral triangle. Complications: bleeding, infection, wound dehiscence, necrosis, lymphocele, lymphoedema, groin / limb numbness. This is a morbid procedure. The modified approach (sparing of the saphenous vein) reduces the rate of lymphoedema to 10-36%.






