As many trainees will know, and I count myself among them, there are a plethora of organisations involved in our training. Most of us will be familiar with our deaneries, the haven we return to once a month for our teaching days either side of a horrendous set of on calls.
Perhaps we are vaguely aware of the Joint Committee on Surgical Training (JCST) who appear at the bottom of our portfolios and send out surveys every once in a while. Even the General Medical Council (GMC) have some sort of role to play… I think?
When I was asked to write an article explaining the interplay between all of the ‘stakeholders’ (a word that seems to be banded around more and more on Microsoft Teams meetings these days) I have to admit, I was none the wiser.
Which is strange when you think about it. After all, these people decide what my job is day to day. How many theatre sessions should I be getting each week? Which far flung district general hospitals might I end up in? What hoops could I be required to jump through to gain my Certificate of Completion of Training (CCT) in the (probably distant) future?
Thinking a bit further than the end of my own nose, these groups have an important role to play in future healthcare planning too. Ultimately, the quality and quantity of urology consultants that the UK produces is down to them.
Some casual googling didn’t really help much. Wikipedia told me that Health Education England is an executive non-departmental public body of the Department of Health and Social Care. Its function is to provide national leadership and coordination for the education and training within the health and public health workforce within England.
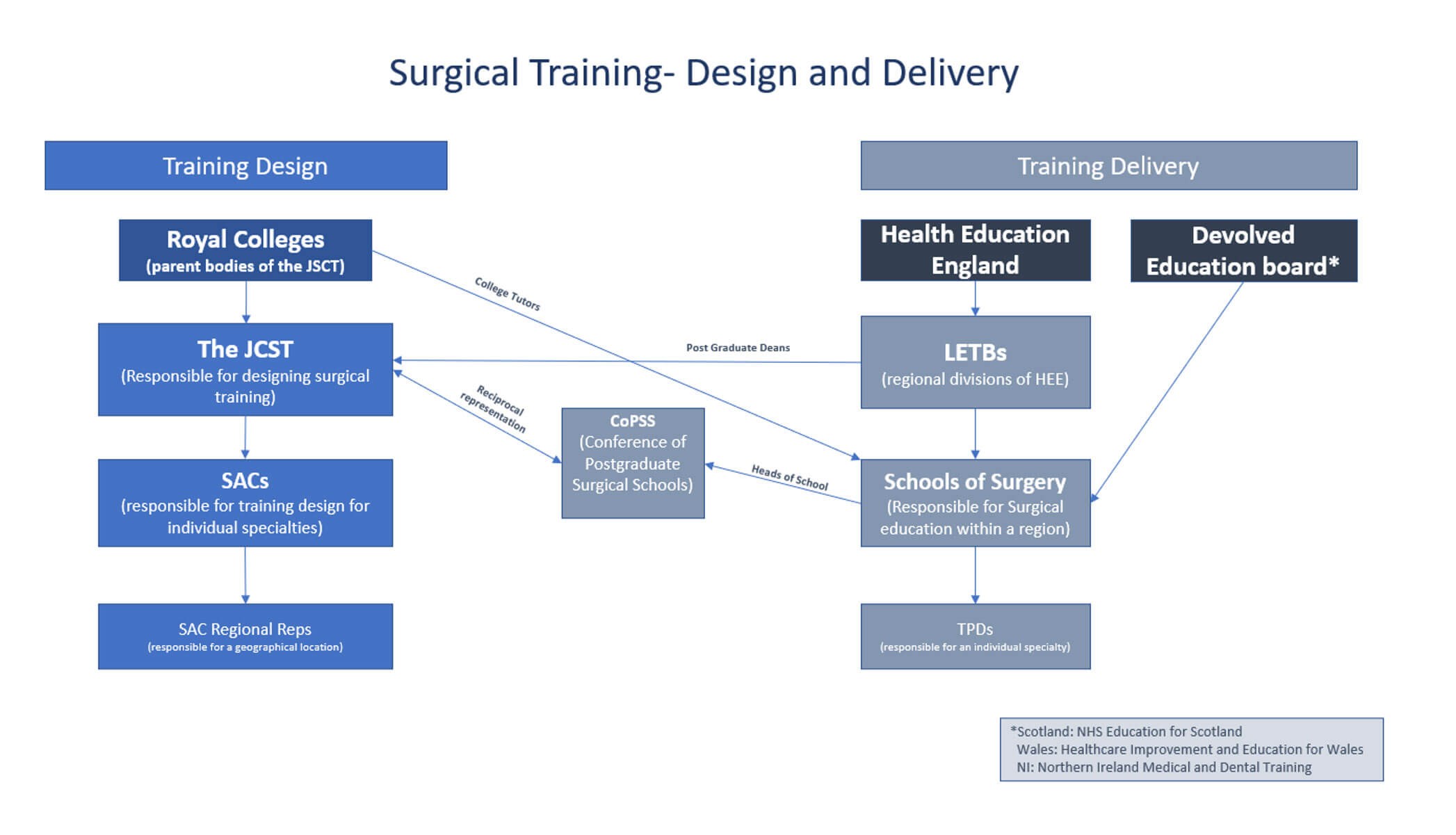
Meanwhile, the JCST website informed me that “The JCST is the parent body of the Specialty Advisory Committees (SACs) and the Training Interface Groups (TIGs)”. Clearly this was going to require some more detailed research. The kind of detailed research that has taken me to the depths of ‘The Gold Guide: A Reference Guide for Postgraduate Foundation and Specialty Training in the UK’ and ‘Regulatory Investigations JSCM intercollegiate policy’. I have dutifully waded through these documents so you don’t have to. And here is a summary of what I found:
Design and Delivery
The easiest way for me (and hopefully you) to understand how our training works is to split it into two broad components.
One is our training design – the length, breadth and depth of our training. ‘What does a consultant urologist need to be able to do and know?’; ‘How many TURPs does it take to be competent?’; etc.
The other is its delivery. Ultimately, all of this training needs to be undertaken in NHS hospitals up and down the country. Somebody (or more accurately many individuals) must be responsible for making it happen.
On the design side … working from the bottom up:
Specialty Advisory Committees (SACs)
What are the SACs?
Each of the 10 surgical specialties (see if you can name them all!) as well as the Core Surgical Training Programme has its own Advisory Committee. They all report to a central body: the JCST (see below).
What do the SACs do?
Each committee is dedicated to designing and managing the training of its respective specialty. The urology curriculum was written by the Chair of the SAC for Urology, Professor Phil Cornford (and a number of others).
Other responsibilities include setting the standards for specialty recruitment, managing less than full-time (LTFT) training, and CCT / Certificate of Eligibility for Specialist Registration (CESR).
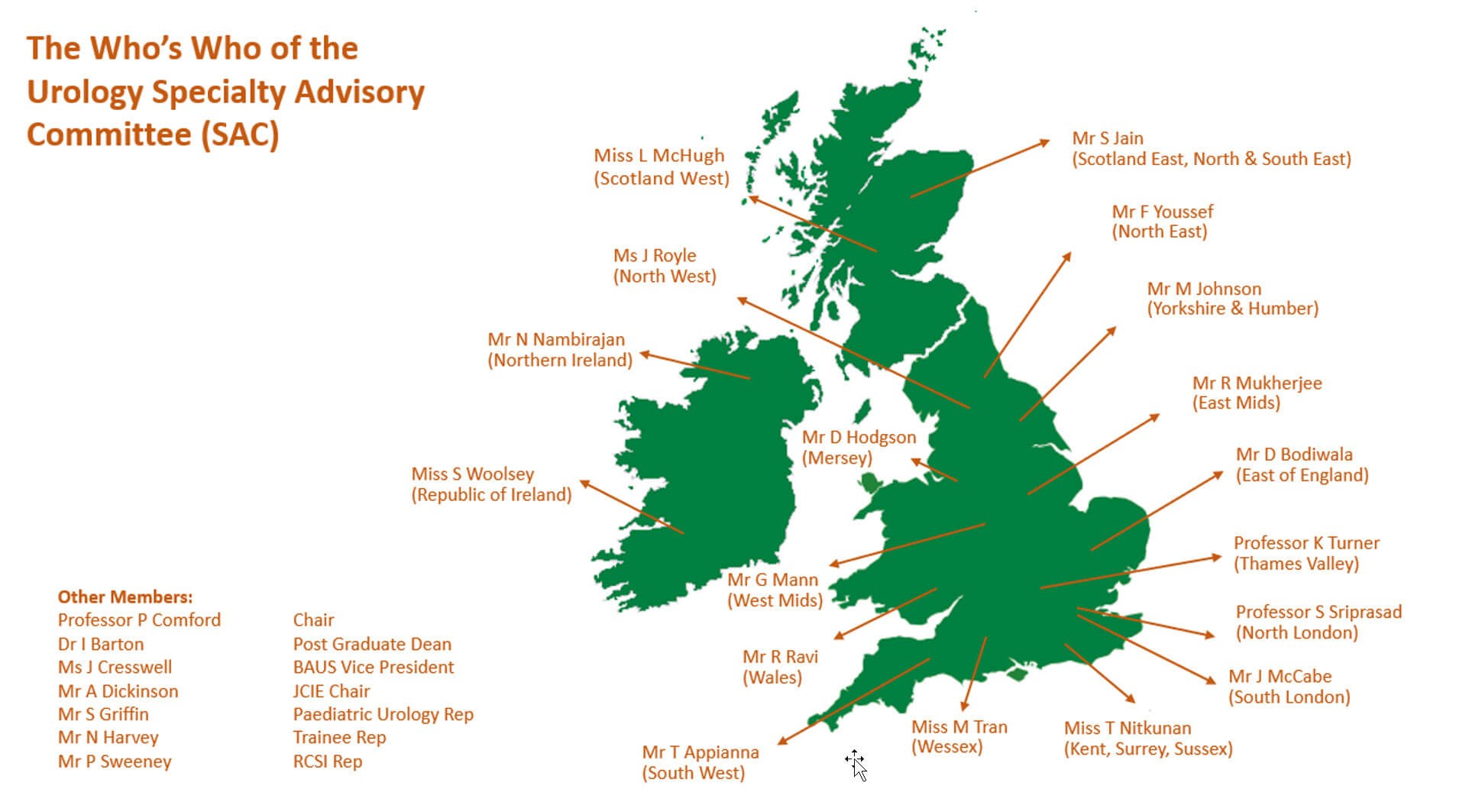
Figure has been adapted from the image file entitled ‘Location map of British Isles’ from Wikimedia Commons
(https://en.m.wikipedia.org/wiki/File:Location_map_of_British_Isles.png). Author Paasikivi, ©2016.
Adapted and reprinted under Creative Commons License (https://creativecommons.org/licenses/by-sa/4.0/deed.en).
Who is part of the SACs?
The majority of an SAC is made up of ‘liaison members’ to roughly correspond to the various UK regions. The number of members directly correlates to the number of trainees in the specialty.
Liaison members are expected to attend annual reviews of competency progression (ARCP), liaise with training programme directors (TPD), and produce annual reports on the state of training in their designated regions.
The remainder of the committee is made up of various other interest groups. For example, the British Association of Urological Surgeons (BAUS) Vice President, Jo Cresswell, sits on the Urology SAC as well as a dedicated paediatric urology representative. It is also mandated that every SAC must include a trainee representative.
And finally, each SAC has a nominated ‘chair’ who in turn sits on the JCST…
The JCST
What is the JCST?
The JCST is an advisory body to the four royal colleges (England, Ireland, Edinburgh and Glasgow) for all things surgical training.
What does the JCST do?
The JCST is the parent body of the SACs. In addition to overseeing and supporting the SACs, the JCST also acts as an interface between the SACs and other key organisations.
The JCST also plays a vital role in holding trusts and schools of surgery (more about them later) accountable to its delivery. The JCST Survey completed by trainees is an important part of this.
Amongst some of its other responsibilities are the maintenance of the Intercollegiate Surgical Curriculum Programme (ISCP) website, conducting research into surgical education and evaluating CCT / CESR applications on behalf of the GMC.
Who is part of the JCST?
The JCST is formed by the SAC chairs as well as representatives from other parties such as the president of the Association of Surgeons in Training (ASiT), the president of both the Membership of the Royal College of Surgeons (MRCS) and Fellowship of the Royal Colleges of Surgeons (FRCS) exam boards and the heads of the postgraduate schools of surgery.
On the delivery side …
Until now, we have discussed the structure of the bodies who design and set standards for our training. The delivery of this training, however, is the responsibility of the various hospitals that we are all sent to. So, this time working from the top, down:
Health Education England (HEE)
At the top of the delivery chain are Health Education England (HEE). HEE is not only responsible for the delivery of education for doctors but all healthcare professionals.
This means liaising with universities, trusts and the Department of Health (their parent body) to ensure the smooth running of the training process of all healthcare professionals.
For those of us training outside of England, each of the devolved nations has its own similar health education board – NHS Education for Scotland (NES), Health Education and Improvement for Wales (HIEW) and the Northern Ireland Medical and Dental Training Agency (NMDTA).
Local education training boards (LETBs)
The deaneries (now officially known as local education training boards or LETBs) are the regional subsidiaries of HEE. Every deanery has a postgraduate dean who must ensure that their LETB trains its doctors from all specialties to standards laid out by the GMC.
They are also tasked with dealing with national issues which are common to all junior doctors such as LTFT training provision and the impact of COVID.
LETBs do not exist in the devolved nations. Scotland has its own equivalent ‘Scotland deanery’ whereas in Wales and Northern Ireland, equivalent responsibilities are shared between their respective health education boards and the schools of surgery.
Schools of surgery (SoS)
The LETBs themselves are further subdivided in ‘schools’ of each specialty. For those outside of England, schools of surgery exist for each of the devolved nations but as there are no LETBs, they report directly to their health education board.
The SoS are responsible for the day-to-day educational experiences of their trainees. Their role is to determine and then agree how the trusts in their region will deliver training in line with guidance set out by the JCST and SACs.
While the setup of each individual SoS varies due to local factors, each will be led by a head of school who works alongside various royal college representatives, trust executives and trainee representatives. Other key members of the SoS are the local surgical college tutors who are directly appointed by the royal colleges.
The SoS are also responsible for the appointment of TPDs who in turn manage educational and clinical supervisors.
Confederation of Postgraduate Schools of Surgery (CPoSS)
Whilst the SoS are managed by their deaneries on a local level, over the whole country they unite under a central organisation: the Confederation of Postgraduate Schools of Surgery (CPoSS).
The CPoSS also offers ‘reciprocal representation’ with the JCST at its meetings, ensuring that those designing training and those delivering it can share ideas.
The GMC
So where do the GMC fit into all of this? The GMC have the overall responsibility for the regulation of our training. In their own words their role is to “secure and maintain standards in postgraduate medical education and training in the UK” as outlined in the most recent edition of Promoting excellence: standards for medical education and training.
But what does this mean in practical terms? Clearly, the GMC has neither the expertise nor the resources to micromanage urology training. It therefore relies on information provided to it by the JCST and LETBs.
On paper, however, it still wields a significant amount of power over training and can get involved in major decisions. For example, all training, urological or otherwise, requires GMC approval to ‘count’ towards eventual CCT. If a trust wishes to be involved in training they must submit an application to the GMC, via their LETB, detailing their suitability. The decision to approve the trust will then be made in conjunction with advice and guidance from the JCST in the form of an ‘endorsement’.
Conversely, should a site fail to reach the standards set out by the GMC, it has the power to impose sanctions and eventually, withdraw its recognition for training. Similar processes exist for completion of training. Although the GMC will ‘rubber stamp’ a doctor’s training to allow them to join the specialist register, it will be the JCST who have ensured that they are competent.
So, there you have it! From SoS to LETB, the A-Z of responsibility for the design and delivery of our urology training.