We are delighted to introduce something new for the Uroradiology Focus – our very own Jane Belfield has put together a urology imaging quiz with 10 cases designed to grab your interest and test your knowledge. Good luck and let us know how you get on!
(Answers at the bottom of the page)
Case 1
A 39-year-old female presented with recurrent urinary tract infection and underwent ultrasound of the renal tract and bladder.
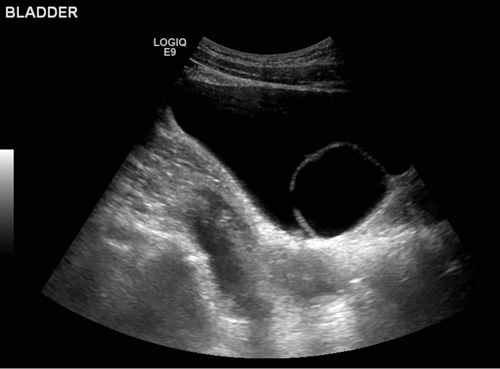
1. Describe the findings.
2. What is the differential diagnosis?
3. What appearance might you see in the upper tracts?
Case 2
A 25-year-old male with previous orchidopexy presented for a testicular ultrasound. A single image is shown below.
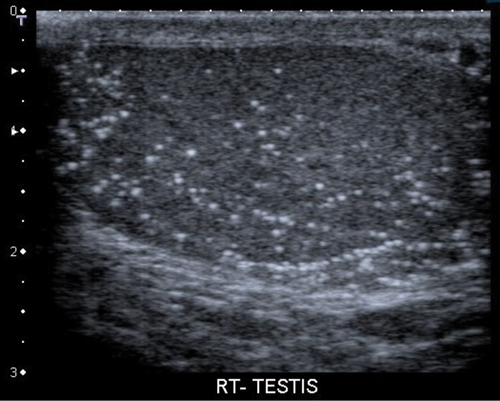
1. Describe the finding on the image.
2. What is the diagnosis?
3. What is the US definition?
4. What further management would you recommend?
Case 3
A 42-year-old female patient.

1. What radiological examination has been undertaken?
2. Describe the findings on the image.
3. What is your diagnosis?
Case 4
A 52-year-old male was admitted following a fall.
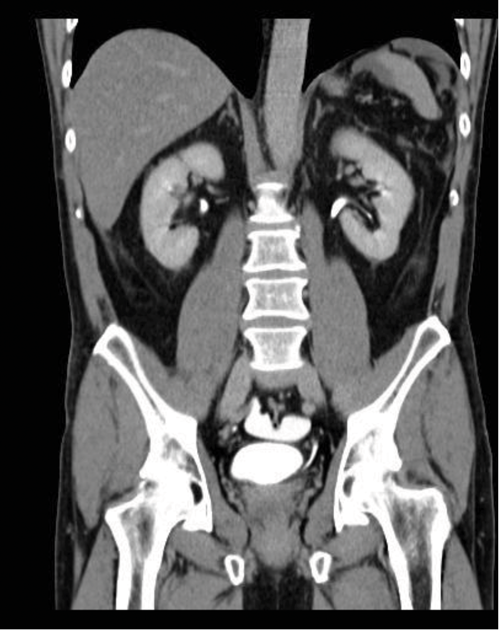

1. How has the CT been performed?
2. Describe the findings.
3. What is the diagnosis?
4. What management is usually required?
Case 5
A 45-year-old male is found to have an incidental right adrenal lesion on CT. An MRI was arranged for further evaluation.
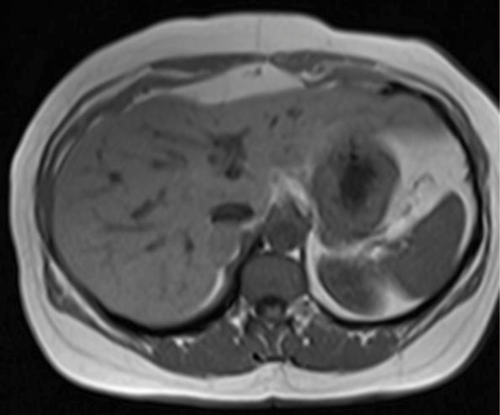
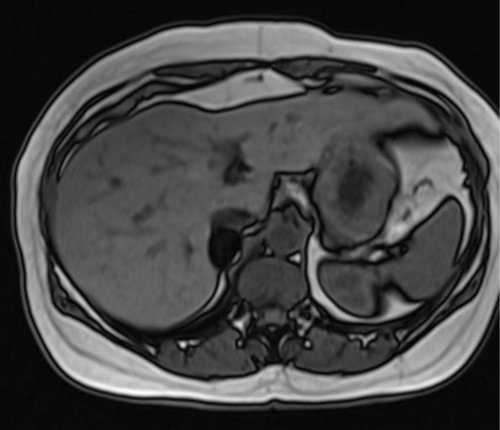
1. What sequences are shown?
2. Describe the findings.
3. What is the likely diagnosis?
Case 6
A 70-year-old male presented with a prostate specific antigen (PSA) of 5.2 and had MRI of the prostate.
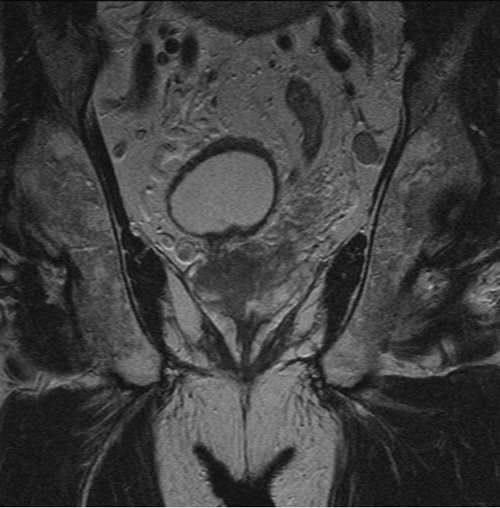
1. What sequence and plane is the MRI image?
2. Describe the findings.
3. What is the radiological staging from the image shown?
Case 7
A 35-year-old female patient attended for investigations.
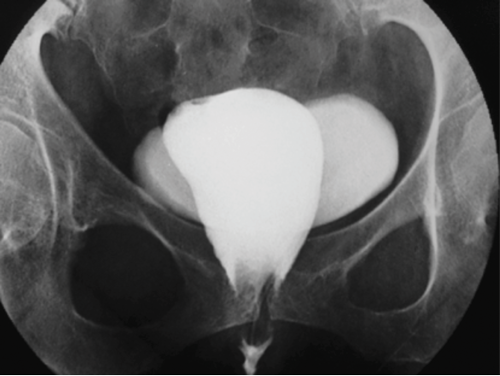
1. What investigation has been performed?
2. Describe the findings.
3. What is the diagnosis?
4. What treatment is usually required?
Case 8
A 20-year-old male presented with a palpable lump for testicular ultrasound.
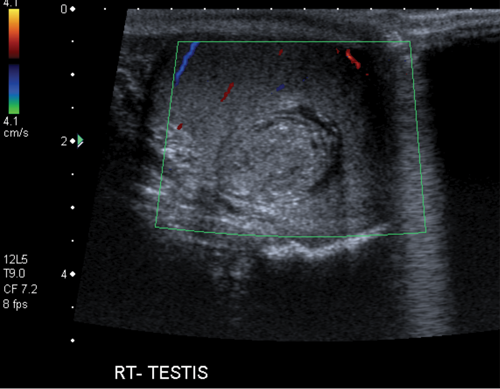
1. Describe the findings on the ultrasound.
2. What is the likely diagnosis?
3. What management would you recommend?
Case 9
A 42-year-old male presented with sepsis, fatigue and abdominal pain. He had a previous history of renal calculi. A contrast CT was performed to ascertain the cause of the pain.
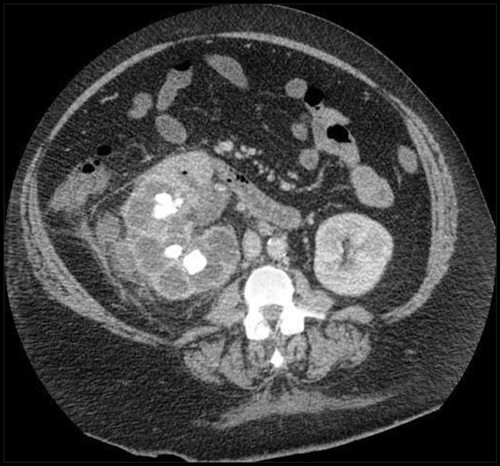
1. Describe the abnormalities seen on the CT.
2. What is the classic description given to this appearance?
3. What is the diagnosis?
4. What treatment is usually required?
Case 10
A 75-year-old male patient attended for radiological investigations two years following cystectomy for bladder malignancy.
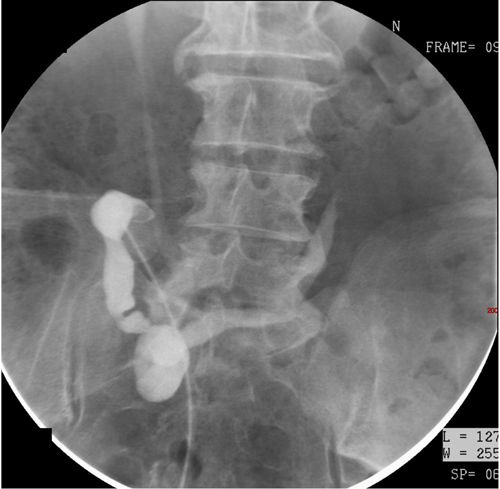
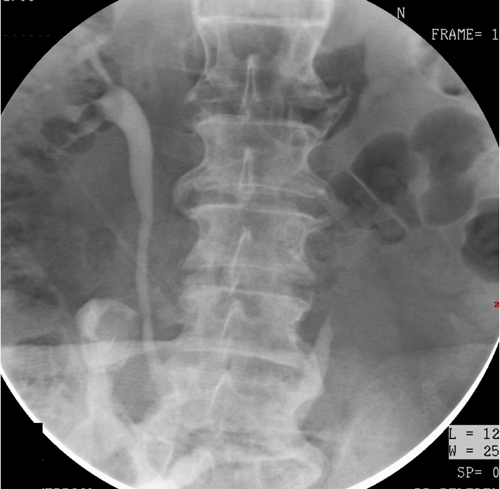
1. What is the radiological investigation?
2. Describe the findings.
3. What is the differential diagnosis?
4. What would you do next?
Answers
Case 1
- There is a well-defined, curvilinear structure seen within the urinary bladder, which contains fluid.
- This appearance could be due to a Foley catheter, foreign body or ureterocele.
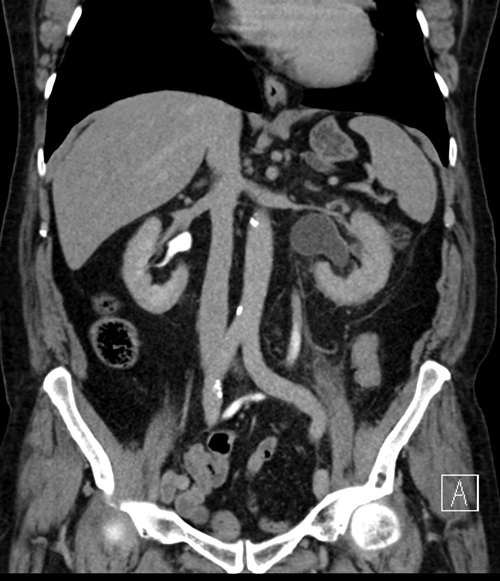
- If the ureterocele is large, the kidney may be hydronephrotic and the ureter dilated all the way down to the bladder. The CTU image below from the same patient demonstrates the ureterocele, and the left kidney is markedly hydronephrotic with hydroureter down to the bladder.Ureteroceles are associated with duplex kidneys, so it is important to assess the affected kidney to ascertain if there are one or two ureters.
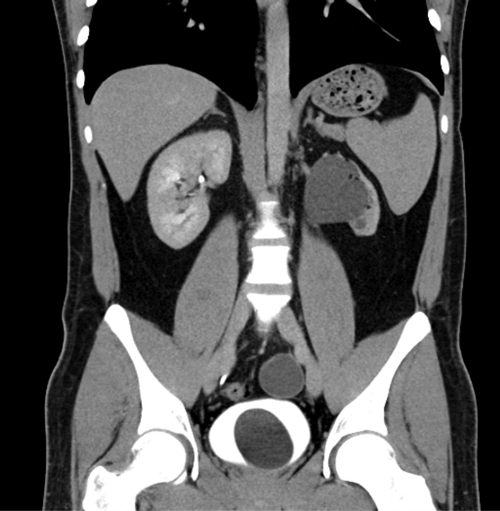
Case 2
- There are multiple hyperechoic foci seen throughout the testis with no posterior acoustic shadowing.
- Testicular microlithiasis.
- Five or more microcalcifications on a single ultrasound image.
- As the patient had previous orchidopexy and has microlithiasis, he is at increased risk of germ cell tumour. Annual ultrasound surveillance is therefore recommended until he is aged 55 years. European guidelines were published in 2015 regarding surveillance of testicular microlithiasis, and annual ultrasound is advised in patients with an independent risk factor for germ cell tumour until the age of 55 years. In patients with no other risk factors, regular self-examination is advised and ultrasound can be performed if a focal lesion is palpated.
Case 3
- A cystogram has been performed. Although the image looks like an intravenous urogram (IVU), the bladder is too densely opacified with contrast for this to be part of an IVU series. The bladder has been distended with contrast during the cystogram.
- Dense opacification of the urinary bladder is seen, which has a smooth outline and appears normal. Contrast is seen to reflux into both ureters and collecting systems which should not be seen as part of a routine cystogram.
- The patient has marked reflux (grade 4). Reflux is graded from 1 to 5, as below:
- Grade 1 – reflux limited to the ureter
- Grade 2 – reflux up to the renal pelvis
- Grade 3 – mild dilatation of the ureter and pelvicalyceal system
- Grade 4 – tortuous ureter with moderate dilatation
- Grade 5 – tortuous ureter with severe dilatation of ureter and pelvicalyceal system. Loss of fornices and papillary impressions.
Sometimes, reflux is not seen during a routine cystogram, but if there is clinical suspicion, further images should be obtained during micturition to assess for mild reflux.
Case 4
- A CT urogram has been undertaken with contrast seen in both collecting systems. A CT cystogram was performed at the same time, with contrast instilled into the urinary bladder via existing Foley catheter. This allows assessment of both the upper tracts and the bladder to look for any injury following trauma. Contrast should be used at a concentration of 10% during CT cystogram, otherwise the contrast opacification will be too dense and make interpretation difficult.
- There is abnormal contrast opacification seen superiorly to the urinary bladder, within the peritoneal cavity.
- Findings are in keeping with an intraperitoneal bladder rupture. This is seen in approximately 15% of major bladder injuries and is usually caused by direct trauma to a distended bladder. The axial CT image demonstrates fluid, some of which has opacified with contrast, in the peritoneum.
- Surgical repair is required for intraperiteonal bladder rupture. Extraperitoneal bladder rupture is more common, accounting for 80-90% of cases, and is usually due to penetrating trauma or as a result of pelvic fractures. Treatment of an extraperitoneal bladder rupture is conservative, with a Foley catheter left in situ until the rupture heals.
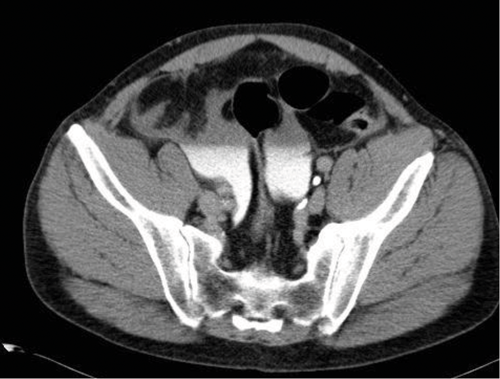
Case 5
- T1 weighted axial MRI in-phase and out-of-phase. Fluid is dark on T1 images, and the cerebrospinal fluid (CSF) in the spinal canal is seen to be dark. When assessing for the type of sequence, looking at vessels can be misleading as they are usually dark due to flow void.
- There is a well-defined nodule seen in the right adrenal gland. It appears solid on the in-phase image and demonstrates complete loss of signal on out-of-phase image.
- The diagnosis is an adrenal adenoma. Loss of signal on out-of-phase imaging is due to chemical shift artefact, caused by the composition of the lesion. An adenoma contains intracellular fat, which causes the loss of signal. It is not composed of macroscopic fat, otherwise it would be bright on both T1 and T2 MRI.
Case 6
- Coronal, T2-weighted MRI. Fluid is bright on T2 and dark on T1 MRI. The bladder can clearly be seen on this image and is bright.
- Low signal is seen predominantly in the right lobe of the prostate and there is bulging of the capsule. Seminal vesicles are not clearly seen on this image so it is difficult to comment on whether they are involved. There is a round, enlarged lymph node in the left hemi-pelvis.
- Radiological staging from this image alone is T3a, N1, M0. There is bulging of the capsule and extracapsular disease, and the left pelvic lymph node has typical appearance of a metastatic node. There is no fatty hilum, it is enlarged and is rounded rather than ovoid. Bone involvement is difficult to accurately assess on T2 MRI and T1 images should be evaluated to assess the pelvic bones and lower lumbar spine.
Case 7
- A cystogram has been performed.
- Contrast is seen to opacify the urinary bladder as well as another structure which has a more longitudinal appearance on the image.
- The diagnosis is a vesicovaginal fistula (VVF). In developing countries, the commonest cause is prolonged labour, but in developed countries 90% are seen due to bladder injury following pelvic surgery. Risk factors include previous surgery, diabetes, endometriosis and infection. Patients usually present with leakage of urine into the vagina, causing urinary incontinence.
- Conservative management can occasionally be successful if a VVF is diagnosed within the first few days of surgery and a urinary catheter is left in situ. Alternatively, surgical repair may be necessary, particularly if the VVF is longstanding.
Case 8
- There is a well-defined, anechoic round lesion in the right testis that demonstrates a ring-like appearance.
- The most likely diagnosis is an epidermoid cyst. Epidermoid cysts account for 1-2% testicular masses and usually present in the second to fourth decades. They typically present as a painless mass and are usually 1-3cm in diameter. They are composed of layers of keratinous debris lined with keratinous squamous epithelium, and classically are described as having an ‘onion-skin’ appearance.
- Although these are benign, there is a very small potential of the lesion being malignant and therefore excision is advised. This can be localised rather than a full orchidectomy being required.
Case 9
- There is right hydronephrosis and perinephric fat stranding adjacent to the right kidney. Air is seen in the collecting system and there are multiple calculi in the right kidney.
- The appearance has a description of a ‘bear’s paw’.
- The diagnosis is xanthogranulomatous pyelonephritis. This is seen in a chronically infected, obstructed kidney, and 80% of cases have renal calculi. The commonest causative organisms are Proteus and E coli. It is often associated with diabetes, or seen in immunocompromised patients. It usually affects the whole kidney, but 15% of cases can be focal.
- Antibiotics should be given, but surgical treatment with nephrectomy is usually required. The affected kidney is usually non-functioning, and patients are often systemically unwell due to the chronic nature of the condition.
Case 10
- This is an ileal conduitogram, where 8F Foley catheter is inserted into the ileal conduit and contrast injected by hand. The ileal loop, anastomosis, both ureters and collecting systems should opacify and be evaluated.
- The ileal loop and anastomosis are clearly seen. The right ureter and collecting system appear normal, with no filling defect seen. The distal left ureter is seen, but the left collecting system and proximal ureter are not visualised.
- This appearance could be due to a stricture, or tumour recurrence in the left ureter.
- The patient needs further evaluation to assess if the left kidney is hydronephrotic and if there is a left ureteric tumour. Ultrasound could be undertaken whilst the patient is in the radiology department to look for hydronephrosis, but CTU would be recommended for full evaluation. An image from the patient’s CTU is shown below, demonstrating left hydronephrosis and a mid ureteric tumour, accounting for the findings on the ileal conduitogram.