Case 1
A 70-year-old female presented under the medical team with malaise, weight loss, and deranged liver function tests (LFTs) and calcium (ALP 350, GGT 650, Serum bilirubin 29, normal aminotransferases, Ca 3.3). An abdominal ultrasound scan (USS) was performed which demonstrated hepatosplenomegaly and an incidental finding in the kidney. A CT was arranged (Figure 1).
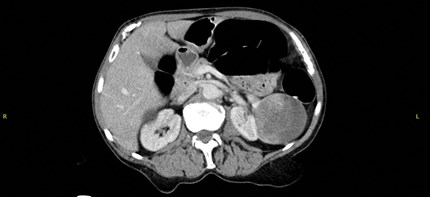
Figure 1.
What does the CT in Figure 1 show?
- What are the salient phases for optimal CT image acquisition for suspected renal cell carcinoma (RCC)?
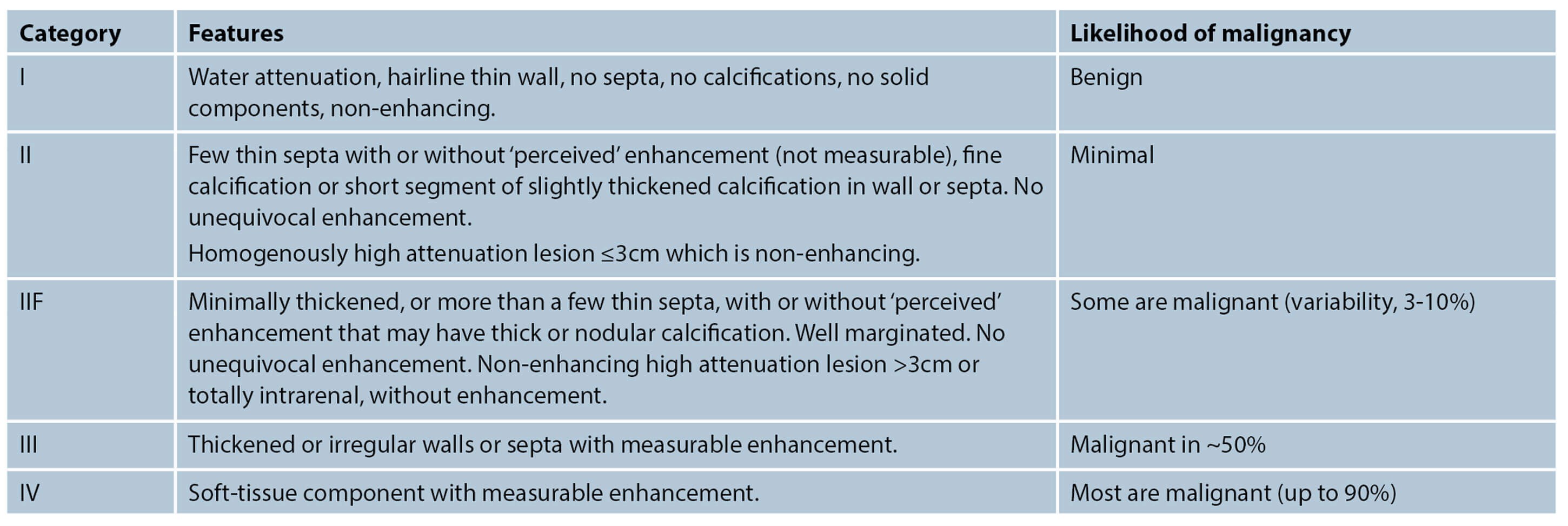
- What is the most widely used CT classification system for renal cystic masses, and what are the features of each category?
- The patient’s staging scans showed no evidence of metastatic disease. What is the likely cause for her deranged LFTs?
- What paraneoplastic syndromes are associated with RCC, and how are these treated?
Case 2
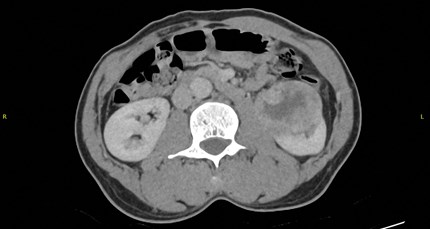
Figure 2.
- What does Figure 2 show?
- What are some of the current proven risk factors for RCC?
- How common is hereditary RCC, and what are the most common causes?
- The above patient subsequently undergoes surgery, and his histology demonstrates clear cell RCC pT2aN0,M0. What prognostic scoring systems may be used to plan his follow-up? What information would be required to score him?
Case 3
A 73-year-old gentleman presented under the general surgical team with abdominal pain. A CT scan was performed (Figure 3) owing to significant tenderness.
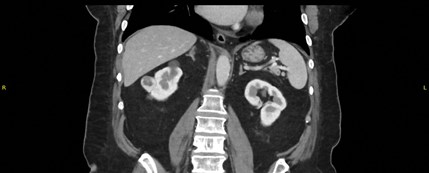
Figure 3.
- What does Figure 3 show?
- Assuming the patient has a performance status of 0 and no significant comorbidities, what options are available?
- What are the indications for nephron-sparing surgery?
- What is the role of biopsy in patients with renal lesions?
Renal masses: answers
Case 1
1. A large cystic mass within the left kidney.
2. The renal mass protocol refers to multi-phasic contrast-enhanced imaging, typically comprising a non-contrast scan (useful for masses containing fat or to determine the HU of homogenous renal masses), cortico-medullary phase (at 30 seconds, best to further delineate subcategories of renal cell carcinomas), nephrogenic phase (80-100 seconds, for optimal enhancement of the renal parenchyma and demonstrate enhancing components of a mass), and excretory phase (around 8-10 minutes, to enhance the calyces, renal pelvic and ureters) [1].
3. Bosniak classification of cystic renal masses. A new updated Bosniak classification was proposed in 2019 with the purpose of including MRI features and to increase accuracy. However, it is still awaiting widespread validation [2-4].

4. Non-metastatic hepatic dysfunction (Stauffer syndrome). The typical picture is that of deranged LFTs in keeping with cholestasis, with raised serum alkaline phosphatase (ALP), elevated prothrombin time, and less commonly elevated serum bilirubin or transaminases. Hepatic dysfunction resolves following nephrectomy in up to 70% of cases, with persistence indicating viable tumour remaining [3].
5. Paraneoplastic syndromes occur in up to 30% of patients with symptomatic RCC. They include the aforementioned Stauffer syndrome, hypercalcaemia (up to 13%), hypertension, polycythaemia, Cushing syndrome, hyperglycaemia, galactorrhoea and clotting disorders [4]. Treatment is via treating the tumour with surgical excision or systemic therapy, aside from treatment of hypercalcaemia with fluid hydration and bisphosphonates [4,5].
Case 2
1. A 7.7cm tumour in the left kidney.
2. Tobacco exposure, obesity, hypertension, and diuretics and other antihypertensive medications are commonly implicated. Others include end-stage renal disease, certain familial syndromes such as tuberous sclerosis, regular use of nonsteroidal anti-inflammatory drugs, and family history. Although predominantly a disease of older adults, the incidence in younger adults has increased [3,4].
3. Three to eight percent of RCC are hereditary [3,4,6]. Familial syndromes associated with renal carcinoma include von Hippel-Lindau syndrome (VHL), hereditary papillary RCC (HPRC), Birt-Hogg-Dubé syndrome (BHD), tuberous sclerosis complex (TSC), hereditary leiomyomatosis and renal cell cancer, succinate dehydrogenase-related RCC, hereditary BAP1-associated RCC, phosphatase and tensin homolog (PTEN) hamartoma syndrome, constitutional chromosome 3 translocations, familial non-syndromic clear cell RCC, renal medullary carcinoma (hereditary haemoglobinopathy association) [3,4,6].
4. Several prognostic scoring systems have been developed for localised clear cell RCC. These include the Leibovich (Mayo) Score / prognostic model (2003) which is used to stratify patients into low-risk, intermediate-risk and high-risk groups. Five risk factors are employed which include tumour, nodes and metastases (TNM) scores, tumour size, grade, and tumour necrosis. The more recent Leibovich score (2018) may be applied to chromophobe RCC, papillary RCC and clear cell RCC [3]. The UCLA Integrated staging system (UISS) and GRANT models may be applied to all subtypes [3].
Case 3
1. A small mid-right partially exophytic enhancing renal mass.
2. All options: active surveillance (AS), surgery (partial nephrectomy or radical nephrectomy), minimally invasive therapy (radiofrequency ablation or cryotherapy).
3. Absolute: solitary kidney or bilateral disease. Relative: impaired renal function in the contralateral kidney, hereditary syndromes with increased risk of future tumours. Elective: localised unilateral RCC with normal contralateral kidney [3].
4. Biopsies are indicated in patients with atypical lesions, patients with metastatic RCC prior to systemic treatment, as well as patients planned for AS, or ablative therapy. In addition, biopsies are considered for those with solitary kidney or bilateral lesions [3].
References
1. Sohaib A, Cook P. Renal and adrenal tumours. In: Nicholson T (ed). Recommendations for cross-sectional imaging in cancer management, Second edition. London, UK; The Royal College of Radiologists; 2014.
2. Silverman SG, Pedrosa I, Ellis JH, et al. Bosniak classification of cystic renal masses, version 2019: an update proposal and needs assessment. Radiology 2019;292(2):475-88.
3. Ljungberg B, Albiges L, Bedke J, et al. EAU Guidelines on Renal Cell Carcinoma 2021.
https://uroweb.org/wp-content/
uploads/EAU-Guidelines-on-Renal-Cell
-Carcinoma-2021.pdf
[Accessed 3 February 2022].
4. Campbell SC, Lane BR. Malignant Renal Tumours. In: Wein AJ, Kavoussi LR, Partin AW, et al. (Eds.). Campbell-Walsh Urology 11th Edition Philadelphia, USA; Elsevier; 2016: 1318-25.
5. National Institute for Health and Care Excellence (NICE). Scenario: Hypercalcaemia – known malignancy [Internet] 2019
https://cks.nice.org.uk/topics/
hypercalcaemia/management/
known-malignancy/
[Accessed 3 February 2022].
6. Maher ER. Hereditary renal cell carcinoma syndromes: diagnosis, surveillance and management. World J Urol 2018;36(12):1891-8.






