It was gutting to miss out on urology at national selection on my first attempt. The ST3 application has become increasingly competitive and this means more appointable trainees find themselves looking to plan B. The options available can be daunting as the opportunities they provide will potentially impact on success in any future applications.
Like most trainees, I left core surgery comfortable with the ‘indicative’ procedures required for ST3 and I was wary of jobs that would shoehorn me into a role that wouldn’t expand on that. I wanted a new experience and a fresh start and one in which I would get ample opportunities to build my portfolio and improve my chances of getting a number.
Thankfully I stumbled across an advertisement for a senior clinical fellow at the transplant surgery department at Guy’s Hospital in London. I knew urology trainees that had rotated through transplant and spoke very highly of their experiences. I wanted more experience in big open operations and didn’t see many opportunities for that in regular urology, especially as an inexperienced staff grade. This was my first proper medical job interview outside of training.
Even as a student, I had no experience of transplant surgery and I had not done a lot of research about it before the interview. I had no experience of renal medicine. I had never worked in a tertiary hospital or in London. I had minimal vascular and open surgical experience. All of the other staff grade registrars in the department were experienced surgeons who had completed training in other countries. Unlike other interviews I attended, nobody else unsuccessful at urology national selection was applying and thankfully my CV, enthusiasm and comfort with basic urology procedures gave me enough edge to be offered the job.
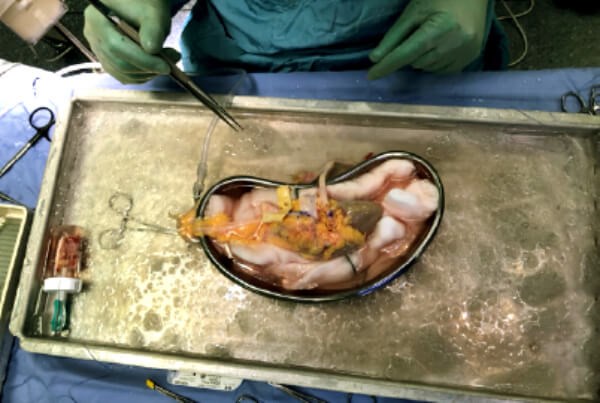
‘Benching’ a deceased donor kidney before transplantation: another opportunity to develop open surgical skills.
Guy’s transplant department perform a lot of operations and it is by far and away the busiest unit I have ever worked in. They perform paediatric and adult kidney transplants (more than any other unit in the UK), simultaneous pancreas kidney (SPK) transplants, living donor nephrectomies along with numerous dialysis access, urological and general surgical procedures. The department operates across multiple sites for 24 hours seven days a week. Compared to urology, the on-calls are intense, with complicated operations happening at all times through the night and weekend. This is great as the registrars are always busy in theatre and assistance is appreciated so the skills of the juniors are developed.
SPK transplant is a truly unique experience in surgery, lasting for as long as 10 hours and starting at any time. Numerous vascular, bowel and urological anastomoses are coordinated between four surgeons on one case after maximum exposure of the great vessels in the abdomen is obtained. Occasionally the entire surgical team rotates during the procedure which is not something I’d ever seen before. It was a privilege to assist on almost 10 SPK transplants in one year and you would be hard pressed to find an operation which provides better training experience for a junior surgeon.
“I had the opportunity to work in a disciplined and highly motivated unit where I was pushed to reach the same standards”
For organ retrieval, there were also opportunities for registrars to join the King’s team. Seeing a living donor kidney perfuse and produce urine intraoperatively is a unique experience and even the excitement of feeling a thrill on your first vascular anastomoses is a perfect way to reignite any enthusiasm for surgery that may have been lost in the national selection process.
I had not done a lot of open surgery going into the job and there was a learning curve to anticipate correctly and assist during a transplant. I could not say at the beginning that I was able to tie at depth efficiently and understand all the different anastomosis techniques used by the different surgeons. It was not easy but by the end of the job, every consultant was comfortable operating with me and I had performed a number of anastomoses myself.
Compared to spending too much time in a flexible cystoscopy clinic and consolidating already developed skills, the opportunity to have a learning curve at something completely fresh is something I would recommend any trainee in a similar situation to look for. Trainees in urology are often working alone. Missing out on a training number takes an emotional toll which a trainee needs to rebuild from. I would say there is a great benefit in working together with very talented and experienced colleagues on cases with regular feedback on your strengths and weaknesses.
For urology trainees considering a year in transplant, Guy’s have two consultants who are also urologists – Mr Jonathon Olsburgh and Miss Rhana Zakri. As well as fulfilling their transplant responsibilities, they perform core urology procedures and take tertiary referrals from far and wide for complex issues.
The department normally has a trainee who does urology on-call, and a urology themed CT2 trainee. I was able to take responsibility for the stent removal service and help Miss Zakri with a regular specialist urinary tract infection (UTI) clinic for transplant patients. The consultants are committed to training and there is support available for audit, interview practice and research. There is a close link to the urology department, which I found great for education and networking. I was kindly invited to a formal ST3 interview course free of charge. There were opportunities to write publications and obtain management experience to make up the portfolio points I was lacking.
I was eventually successful on my second attempt and am now taking up a number in the East of England deanery. With the benefit of hindsight, missing out on a number was a good thing to happen for my career. I was able to pursue an incredible surgical experience that I may never have got. Knowledge of renal medicine and kidney transplantation is relevant to urologists and certainly was an area I was lacking. I had the opportunity to work in a disciplined and highly motivated unit where I was pushed to reach the same standards. I was able to assist on more than 40 kidney transplants as well as complicated reconstructive urological procedures.
I now feel comfortable with open surgery and my horizon has broadened in unexpected directions. I have seen major haemorrhage managed multiple times by different people and had experience in closing small arteriotomies myself. Even my technique with basic procedures was refined to a demanding standard over months. I personally needed the push working a transplant job provides and I imagine many trainees missing out on a number at ST3 are the same. I was surprised I was not in competition with the faces that became familiar at other interviews. Many urology trainees don’t realise that transplant urology is an area that will provide them with professional development and even a potential career.
Compared to what I heard from peers working in similar situations, I can say the opportunities on offer at Guy’s as a senior clinical fellow in transplant are unparalleled in terms of operative exposure, interview and portfolio support, and life experience at a hospital in central London. I would strongly recommend applying to any trainee missing out on a ST3 number.