This article has been verified for CPD. Click the button below to answer a few
short questions and download a form to be included in your CPD folder.
Flexible ureteroscopy (f-URS) has become a core modality in the treatment of renal calculi, offering high success rates, minimised invasiveness, and a broad scope of application across various patient populations. Driven by continuous technological innovation and procedural refinements, f-URS is increasingly favoured over extracorporeal shockwave lithotripsy (ESWL) and, in select cases, percutaneous nephrolithotomy (PCNL), especially for stones under 2cm.
Recent literature highlights advancements in single-use scopes, suction-assisted access, digital optics, and laser technology. Furthermore, improvements in safety, cost-effectiveness, and expanded indications in special populations have made f-URS one of the most transformative areas in modern endourology [1–3].
Technological advancements
Suction systems in flexible ureteroscopy
Suction-integrated flexible ureteroscopy (s-URS) represents a recent technological advance aimed at improving stone clearance, reducing operative time, and minimising complications such as high intrarenal pressure (IRP) or postoperative infection. This is particularly invaluable during dusting and basketing, as suction systems facilitate continuous fragment evacuation and IRP regulation [1,2].
Suction URS uses specialised ureteral access sheaths with built-in suction ports, such as tip-bendable suction access sheaths, modified access sheaths connected to suction pumps, and dual-channel scopes with separate suction ports [4]. The fluid pathway is important to facilitate controlled inflow irrigation, combined with regulated outflow suction, to maintain a low-pressure system that improves visibility and fragment retrieval.
Several studies have shown its efficacy. A randomised controlled trial (RCT) showed that suction incorporated f-URS was found to be non-inferior to mini PCNL for 2–3cm stones [4]. A stone-free rate of 95.6% at day 30 and reduction in operative time was noted in one study [5]. Rates of s-URS and standard URS are compared in Table 1.

Suction systems extend the scope for f-URS with stones >1.5cm and clinical trials are ongoing to compare with mini PCNL on the efficacy and complication rates [6]. In the future we may expect to see smart pressure-controlled suction pumps, integrated suction channels within digital ureteroscopes, and AI-driven fluid dynamics for real-time IRP monitoring.
Single-use vs. reusable flexible ureteroscopes
Sterilisation of reusable scopes involves complex, multi-step processes (high-level disinfection, mechanical cleaning), which can be error-prone and associated with biofilm formation and cross-contamination [7]. Advantages of single-use scopes are the eliminated risk of contamination and reduced surgical delays from sterilisation, so it is therefore recommended for immunocompromised, pregnant, or infected patients [8–10].
A 2024 study found detectable contamination in 13% of reusable ureteroscopes even after reprocessing [7]. Multiple prospective studies and reviews have reported non-inferior stone-free rates (SFRs) and complication profiles when comparing single-use and reusable f-URS (Table 2).
Cost-effectiveness
This remains one of the most debated areas, and cost-efficiency depends heavily on many factors (Table 3).
Surgeon experience and scope ergonomics
Surgeon feedback varies by device. Single-use scopes are generally lighter, have newer deflection mechanics, and consistent performance, so are preferred in training and remote settings. The advantages of reusable scopes are better tactile feedback, smoother irrigation, and better visualisation thus are preferred in complex anatomies or long procedures [14–16]. A worldwide survey by Dauw et al. in 2015 noted that 92% of surgeons felt scope familiarity impacted their performance more than scope type [15].
Laser lithotripsy evolution
The holmium:YAG laser remains the main method used in lithotripsy. However, the thulium fibre laser (TFL) offers lower retropulsion, faster ablation rates, and greater control in dusting and popcorning modes [17–19]. Meta-analyses confirm that TFL provides superior outcomes in complex or large stone burdens [18].
Holmium:YAG laser: the established modality
Ho:YAG laser works at 2120nm, which is strongly absorbed by water. The laser causes photothermal ablation, leading to vapour bubble formation that fragments calculi on contact.
The main advantages of Ho:YAG is the applicability to all stone types and compositions. The risk of ureteral injury is also minimal and there are a wide range of fibre diameters that are compatible with most available scopes.
The main drawback of Ho:YAG laser is the high retropulsion – it can displace smaller fragments during lithotripsy, reducing stone-free rates. It is less effective for fine dusting due to longer pulse durations and higher energy thresholds. Holmium laser requires high energy and cooling infrastructure, thus units are bulky and less portable.
Thulium fibre laser: the emerging challenger
TFL operates at 1940nm, with even stronger absorption in water than Ho:YAG. It delivers lower peak power but with higher frequency (up to 2000Hz), making it more efficient in producing stone dust with minimal mechanical recoil. Several studies have noted greater precision in dusting and popcorning modes and reduced operative time. TFL uses thinner fibres, improving scope deflection and irrigation.
A systematic review comparing TFL and Ho:YAG for renal stone treatment found that TFL resulted in shorter operative times, less retropulsion, and higher fine dust production. No difference was noted in complication rates or ureteral injury risk [1]. The TFL group achieved 94% SFR vs. 89% with Ho:YAG and average operational time was 15% shorter with TFL [2]. TFL was used in larger stones >2cm and found that the laser activation time was less and the reduction in the need for basket retrieval due to better popcorning and dusting.
TFL has been useful for lower pole stones due to providing finer dust with minimal retropulsion. As higher frequencies up to 2000Hz can be used, popcorning is more successful with TFL. However, for fragmentation and extraction, Ho:YAG remains more effective, for basket-heavy procedures [8,20].
Surgeons are now tailoring energy settings based on stone hardness, anatomical location, and preferred clearance strategy.
Initial cost of TFL units is currently higher, but long-term costs may be offset by lower power consumption, less scope wear and tear due to smaller fibres and shorter operating times. Ho:YAG lasers may be more available in legacy centres but are gradually being supplemented or replaced in academic institutions [8,21].
Future directions for the technology include:
- Pulsed and modulated TFL systems for targeted dusting.
- AI-assisted laser settings for automatic stone recognition and ablation control.
- Hybrid fibre platforms to combine both technologies in one unit. Ongoing trials are being conducted to explore TFL use in paediatric and high-infection risk patients, where rapid clearance and minimal irrigation are critical [3].
Stone-free rates in flexible ureteroscopy
A key benchmark for evaluating the success rate of this procedure is the SFR, defined as the complete absence or clinically insignificant residual fragments post-procedure, typically measured at 2–4 weeks postoperatively using imaging modalities like CT or ultrasound.
Stone-free rates by location and stone characteristics
Lower pole stones often show reduced SFR due to difficult access and unfavourable gravity for fragment evacuation [4,5]. However, this can be mitigated by preoperative planning and advanced deflection scopes.
Stone size and volume as predictors
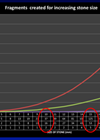
SFRs are highest in stones <10 mm (up to 97%), The SFR reduces gradually with stones >20mm, unless staged or suction-assisted URS is used. Recent studies suggest that stone volume is a more accurate predictor of surgical complexity and outcome than maximum diameter. A study by Knoll et al. demonstrated that 3D volume-based prediction models had higher predictive accuracy for SFRs [22].

Comparison with alternative modalities (Table 4)
Extracorporeal shock wave lithotripsy
ESWL is non-invasive but shows lower SFRs (60–80%), especially for lower pole or dense stones, f-URS achieves superior SFR in both adult and paediatric populations [9,10].
Mini-PCNL
For stones 1.5–2.5cm, mini-PCNL has slightly higher SFRs (~95–98%). f-URS provides comparable outcomes with lower morbidity, shorter hospital stay, and less bleeding [17,18].
Efficacy in special populations
Paediatric patients
Flexible ureteroscopy is increasingly preferred over ESWL in children due to a reported SFRs of 88–94%, lower retreatment rates, and reduced complication rates and long-term ureteral trauma when using miniaturised scopes [10,16].
Elderly and high-risk patients
In elderly, obese, coagulopathic, and pregnant patients, f-URS offers a safer profile than PCNL, comparable SFRs (85–92%) and avoidance of general anaesthesia in selected outpatient cases [17,18].
Outpatient and ambulatory settings
Recent studies support the safety and efficacy of f-URS as a day-case procedure, reporting SFRs of 90–95%, complication rates under 10% and higher patient satisfaction rates [19].
The definition of SFR can vary, however. Some studies use complete absence of visible fragments and others accept residuals <2 mm or clinically insignificant residual fragments (CIRFs). Ongoing research aims to standardise SFR definitions and imaging protocols, incorporate machine learning for predicting surgical outcomes and use automated endoscopic image analysis to detect residual fragments in real time. Advancements in laser technology (e.g., thulium fibre laser) and suction systems are further enhancing the ability to reach and clear difficult stone burdens [18,19].
Complications and prevention strategies in flexible ureteroscopy
Despite its advantages, f-URS is not without risks. Complications range from minor postoperative symptoms to rare but serious injuries such as ureteral avulsion and urosepsis. Prevention requires a deep understanding of procedural mechanics, patient risk profiles, and technology-driven safeguards.
Classification and incidence of complications
Complications following f-URS are typically classified using the Clavien-Dindo system. Most are Grade I–II, but Grade III–V events, though rare, are clinically significant.
Risk factors for complications
Several factors are identified as causes for postoperative complications which include high IRP due to excessive irrigation [6], prolonged operative time (>60 min), large stone burden, absence of preoperative stenting, pre-existing infection or positive urine culture, and inexperience or poor scope handling techniques [7].
Research analysed 432 f-URS cases and found positive preoperative urine culture, operative time >70 minute, and non-use of ureteral access sheaths to be independent predictors of postoperative infection and bleeding [1].
Strategies to prevent complications
Use of ureteral access sheaths (UAS) reduces frictional trauma and scope manipulation injury. UAS results in better irrigation and lower IRP and also improves procedural efficiency and reduces operative time. UAS use has been shown to reduce pyelovenous backflow, thereby decreasing infectious complications [6,8].
High IRP (>40cmH₂O) increases the risk of pyelovenous backflow, hematogenous spread of bacteria and sepsis. This could be prevented by gravity irrigation or low-pressure pumps, suction-assisted ureteroscopy systems and real-time IRP monitoring [6].
All patients must undergo preoperative urine culture and sensitivity testing. Culture-directed antibiotics are superior to empirical therapy in preventing sepsis and it is best to defer surgery until infection resolution is confirmed. A study revealed and emphasised that bacteriuria, even asymptomatic, increases risk of SIRS post-URS [9].
Preventative strategies, from an energy settings and laser technique point of view, suggest the use of pulsed energy modes to reduce thermal damage, avoid prolonged laser activation in confined calyces and choice of dusting over fragmentation in delicate anatomy regions. Thermal damage contributes to delayed ureteral stricture formation [5].
Meticulous surgical technique is imperative in preventing complications. More specifically, it is essential to avoid forceful advancement in non-dilated ureters, to pre-stent in tight anatomy or large stone burden, and to use lubricants and hydrophilic guidewires to reduce frictional trauma [23–26].
Robotic and AI integration in flexible ureteroscopy
f-URS has evolved significantly in the last decade with technological innovation, yet key procedural steps such as scope deflection, manual targeting, and laser activation, still rely heavily on surgeon dexterity and experience. Recently, robotics and artificial intelligence (AI) have begun reshaping this landscape, aiming to enhance precision, reduce surgeon fatigue, and increase procedural consistency.
Rationale for robotic integration
Manual f-URS is technically demanding due to scope torque and fatigue during prolonged procedures, subtle intrarenal navigation challenges and variability in outcomes based on surgeon experience.
Robotic integration offers stabilisation and fine motor control, motion scaling and tremor elimination, and improved ergonomics and remote console operation.
Current robotic URS platforms
A study demonstrated that users (including trainees and urologists) adapted quickly to the Ily® system, even with no prior experience, illustrating its potential for reducing the learning curve in f-URS [26].
Advantages and challenges of robotic systems
Robotic systems improve accuracy and stability during stone targeting, reduce musculoskeletal strain and provide potential for telerobotic surgery and remote case collaboration.
Unfortunately, as with any robotic system with the involvement of AI, the cost is higher and limited in availability. There are scope integration limitations and reduced tactile feedback as compared with manual f-URS.
AI in flexible ureteroscopy
AI and machine learning (ML) technologies are emerging in automated stone detection from endoscopic video frames, intraoperative skill assessment and training evaluation, laser parameter optimisation algorithms, and predictive analytics (e.g., stone-free probability, complication risk, etc.). One such system piloted an automated efficiency score for assessing ureteroscopic skill by tracking hand movement smoothness and laser activation timing using AI. This system showed high agreement with expert ratings [27].
Predictive modelling in URS outcomes
AI models are being trained, using thousands of retrospective case variables to predict SFRs based on preoperative CT scans and to anticipate the need for staged procedures. They also suggest optimal laser energy settings and irrigation patterns. This could lead to personalised procedural planning, especially in complex stone disease or anatomical anomalies.
Robotic-AI synergy: the future of ‘smart endourology’
The convergence of robotics and AI may enable autonomous scope navigation based on preoperative 3D imaging, real-time stone classification and targeting and pressure-based irrigation modulation. Robotic systems integrated with computer vision and AI will play a central role in automating basic tasks during URS, allowing surgeons to focus on decision making and exception handling [8].
Recent advances in AI and robotics are transforming flexible ureteroscopy. AI-based image analysis can assist in real-time stone detection, while robotic scope control platforms reduce surgeon fatigue and enhance accuracy. Smart irrigation systems with pressure feedback further aid in reducing complications such as sepsis and perforation [28].
Future systems are expected to integrate endoscopic vision with predictive analytics to guide energy delivery, optimise laser parameters, and anticipate complications based on intraprocedural data. These innovations promise to personalise treatment and elevate stone-free outcomes across populations.
Conclusion
Flexible ureteroscopy has evolved into a cornerstone of modern endourology, offering a minimally invasive, highly effective method to the management of renal calculi across a broad spectrum of patients. Advancements in scope design – including single-use digital models, suction-enabled access systems, and miniaturised optics – have significantly improved procedural safety, ergonomics, and stone-free rates. Laser lithotripsy, particularly with the emergence of the thulium fibre laser, has redefined efficiency in stone fragmentation, enabling finer dusting with reduced retropulsion and operative time.
Clinical data now supports f-URS as a frontline therapy not only for small-to-moderate stones but also for complex cases, including lower pole stones, paediatric urolithiasis, and high-risk populations.
The integration of robotics and AI promises a paradigm shift in precision, consistency, and surgeon training, offering the potential for semi-autonomous navigation, predictive analytics, and optimised intraoperative decision-making.
However, despite its many advantages, f-URS is not without its complications. Ureteral injuries / avulsion, infection, and postoperative morbidity reiterate the need for continued awareness in technique and patient selection. Preventative strategies – such as controlled irrigation, real-time intrarenal pressure monitoring, and antimicrobial stewardship – must remain integral to best practices.
Looking ahead, integration of AI-assisted technologies, standardised outcome assessments, and global training protocols will be important in further advancing flexible ureteroscopy. As the field moves toward precision-guided, robotic assisted interventions, f-URS is set to remain not just a tool, but a comprehensive platform for the future of stone surgery.
References
1. Wright AE, Rukin NJ, Somani BK. Ureteroscopy and stones: current status and future expectations. World J Nephrol 2014;3(4):243–8.
2. Giusti G, Proietti S, Villa L, et al. Current standard technique for modern flexible ureteroscopy: tips and tricks. Eur Urol 2016;70(1):188–94.
3. He M, Dong Y, Cai W, et al. Recent advances in the treatment of renal stones using flexible ureteroscopy. Int J Surg 2024;110(7):4320–8.
4. Zhu W, Chai CA, Ma J, et al. Flexible ureteroscopy with a tip-bendable suction ureteral access sheath versus mini-percutaneous nephrolithotomy for treatment of 2-3-cm renal stones: study protocol for an international, multicenter, randomized, parallel-group, noninferiority trial. Eur Urol Open Sci 2024;70:167–73.
5. Bai J, Shangguan T, Zou G, et al. Efficacy and intrarenal pressure analysis of flexible and navigable suction ureteral access sheaths with flexible ureteroscopy in modified surgical positions for 2–6 cm upper urinary tract stones: a multicenter retrospective study. Front Med (Lausanne) 2024;11:1501464.
6. Chen KW, Koo KC, Zhong T, et al. Real time monitoring of intrarenal pressures while using the flexible and navigable suction ureteral access sheath. World J Urol 2025;43(1):76.
7. Punga AM, Ene C, Bulai CA, et al. Complications of single-use vs. reusable flexible ureteroscopy. Cureus 2024;16(12):e76256.
8. Juliebø-Jones P, Keller EX, Haugland JN, et al. Advances in ureteroscopy: new technologies and current innovations. J Clin Urol 2022;16(3):190–8.
9. Samir A, El Gamal O, El Gamal S, et al. Safety of single-use flexible ureteroscopy for dusting of upper urinary tract calculi in children. Afr J Urol 2024;30:26.
10. Boston Scientific. Evolving trends lead to unmet needs in flexible ureteroscopy.
www.bostonscientific.com/en-EU/medical-specialties/
urology/stonesmart/smarthub/evolving-trends
-lead-to-unmet-needs-in-flexible-ureteroscopy.html
11. Mille E, El-Khoury E, Haddad M, et al. Comparison of single-use flexible ureteroscopes with a reusable ureteroscope for the management of paediatric urolithiasis. J Pediatr Urol 2023;19(3):248.e1–e6.
12. Skolarikos A, Gravas S, Laguna MP, et al. Training in ureteroscopy: a critical appraisal of the literature. BJU Int 2011;108(6):798–805.
13. Mazzucchi E, Marchini GS, Berto FCG, et al. Single-use flexible ureteroscopes: update and perspective in developing countries. A narrative review. Int Braz J Urol 2022;48(3):456–67.
14. Somani B. Advancements in minimally invasive urology and uro-technology: current status, evolution and future prospects. Ther Adv Urol 2025;17:17562872251329898.
15. Dauw CA, Simeon L, Alruwaily AF, et al. Contemporary practice patterns of flexible ureteroscopy for treating renal stones: results of a worldwide survey. J Endourol 2015;29(11):1221–30.
16. Chen S, Xu B, Liu N, et al. Improved effectiveness and safety of flexible ureteroscopy for renal calculi (<2 cm): A retrospective study. Can Urol Assoc J 2015;9(5–6):E273–7.
17. Mitroi GF, Drăgoescu PO, Mitroi MR, et al. Clinical outcomes and safety assessment of flexible ureteroscopy as an outpatient procedure: a retrospective single-center study. Life 2024;14(9):1131.
18. Akram M, Jahrreiss V, Skolarikos A, et al. Urological guidelines for kidney stones: overview and comprehensive update. J Clin Med 2024;13(4):1114.
19. El-Nahas AR, Elhammadi MG, Abolazm AE, et al. Trifecta in flexible ureteroscopy for treatment of renal and upper ureteral calculi: a multicenter study. Arab J Urol 2024;22(3):166–70.
20. Tang X, Wu S, Li Z, et al. Comparison of thulium fiber laser versus holmium laser in ureteroscopic lithotripsy: a meta-analysis and systematic review. BMC Urol 2024;24(1):44.
21. Awad MA, Johnson BA, Pearle MS. New techniques and technologies in flexible ureteroscopy. J Endourol 2025;39(S1):S8–S17.
22. Panthier F, Alvarez E, Gauhar V, et al. Stone volume instead of maximum stone diameter: results from an international survey. BJU Int 2025;136(1):95–102.
23. Chuang T-Y, Kao M-H, Chen P-C, et al. Risk factors of morbidity and mortality after flexible ureteroscopic lithotripsy. Urol Sci 2020;31(6):253–7.
24. Fonseka T, Melchionna A, De Luyk N, et al. A contemporary step-by-step guide to performing flexible ureterorenoscopy for renal calculi. Curr Urol 2024;18(4):265–7.
25. Karkin K, Alma E, Vuruşkan E, et al. Safety and efficacy of flexible ureterorenoscopy: large series. Cureus 2022;14(3):e23307.
26. Desai MM, Sun Y, Gill IS. Robotic flexible ureteroscopy: the future of stone surgery? Eur Urol 2024;85(1):101–8.
27. Brigham Health. New efficiency score advances the potential for fully automated ureteroscopic skills assessment. 2023.
https://www.brighamhealthonamission.org/
2023/12/27/new-efficiency-score-advances-the
-potential-for-fully-automated
-ureteroscopic-skills-assessment
28. Geavlete B, Mareș C, Mulțescu R, et al. Hybrid flexible ureteroscopy strategy in the management of renal stones - a narrative review. J Med Life 2022;15(8):919–26.
[All Links last accessed September 2025]
Declaration of competing interests: None declared.