For many decades, the condition of giggle incontinence (enuresis risoria, giggle micturition) has remained a rare and poorly understood condition. Patients (90% female) present in their teens, with the history revealing an issue for many years. It is debilitating and causes isolation and low mood, because the very thing patients seek to avoid is laughter.
In fact, several of my patients will describe falling onto puddles on the ground to cover the fact they have lost continence whilst enjoying a joke with friends and ultimately, they remove themselves from social situations. Since its first appearance in the literature in 1959 [1], discussion initially surrounded what constituted a sufficient outburst of laughter to cause leakage. Of course, there are many words to describe various such displays of joy, but agreement has it that it is an uncontrolled, or all-consuming type of laughter, rather than a giggle or titter, which is associated with the disorder. Furthermore, it must be associated with a complete void (not just a dribble which might be expected with stress incontinence). Nevertheless, the word ‘giggle’ has persisted. To diagnose someone, the incontinence must also occur as an isolated experience; in other words, the patient must not show signs of urge or stress incontinence, and a thorough history will determine this.
The aetiology is also a sticking point – the range of treatments each providing some evidence as to the possible cause – and this is still unclear. In short, it is postulated that it may be either a non-neurological or neurological condition. Laughter depends upon complex neurological factors with different neural pathways used in differing stimuli e.g. being tickled compared with finding a joke funny, so also depends upon cognitive factors, but also involves abdominal contraction and the stability of the detrusor, bladder neck and contraction of the pelvic floor [2].
Following thorough history and examination, non-invasive urodynamics and uroflowmetry should take place, utilising ultrasound scan to ensure complete emptying and sensations to void are accompanied by appropriate volumes of urine. My personal practice is to avoid invasive urodynamics until considering centrally acting pharmaceuticals. These investigations should reveal those with non-neurogenic bladder overactivity. As we will see, treatment strategies can overlap diagnoses.
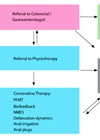
Once the diagnosis of pure giggle incontinence has been made, without any co-existing urge or stress incontinence, discussions about treatment can begin. General principles of good toileting habits, avoiding constipation, keeping the bladder empty with timed voiding and drinking appropriate volumes of water (avoiding caffeinated and carbonated drinks) are of course the first line of any discussion with children with voiding dysfunction. Second is a reassurance that the symptoms become better with age. Anecdotally this is likely true, but probably represents the condition being managed better by a more adult population. Where we move after this is moot, and the most common approaches are discussed below.
"Following thorough history and examination, non-invasive urodynamics and uroflowmetry should take place, utilising ultrasound scan to ensure complete emptying and sensations to void are accompanied by appropriate volumes of urine"
Whereas someone with pure stress incontinence due to poor pelvic floor musculature might dribble when running or jumping, a patient with giggle incontinence may not reach the leak threshold until a great increase in abdominal pressure that comes with uncontrolled laughter. Therefore, treatments aimed at strengthening and accelerating the recruitment of the pelvic floor have been used with apparent success, supporting this theory. Children typically poorly understand the concept of the pelvic floor and biofeedback using visual ‘computer game’ interactions teaches them how to use these muscle groups. Reported long-term success with the lessons learned from biofeedback reaches 94% [2,3] and is strongly recommended to be the treatment strategy prior to pharmacological agents [4].
Reducing the excitability of the detrusor is another target of treatment. Although one might assume overactivity of the bladder would show itself without laughter, the use of direct anticholinergics such as oxybutynin, tolterodine or even imipramine (whose primary role as an antidepressant with anticholinergic side-effects is well known), have been successful in treating this condition, but the evidence is not strong. One study reported an 89% success rate using antimuscarinic medication [5], but many of the patients recruited showed diurnal +/- nocturnal voiding dysfunction beforehand, including urgency, so it is unsurprising that these treatments worked. All the patients reported feeling the sudden urge to void while laughing – in my experience children do not get this feeling – they laugh and the urine flows uncontrollably without any urge. In pure giggle incontinence, one theory is that laughter is accompanied by unstable detrusor contractions, and so antimuscarinics are certainly a reasonable approach as a second line.
Following this comes the more likely, but controversial, theory of giggle incontinence. The similarity to cataplexies, including narcolepsy, cannot be ignored. These conditions involve generalised hypotonia following extreme external emotional stimulus, caused by overactive cholinergic receptors in the basal forebrain resulting in excessive reuptake of acetylcholine [2]. If this occurs at the pelvic floor during laughter, giggle incontinence ensues. So why does it occur in females much more commonly, since it is not associated with a weaker pelvic floor? The fascinating answer to this may lie in functional brain MRI explaining that men and women interpret humour differently [6] – a fact that may come as no surprise to both sexes!
Pharmacologically, it may be the result of an increase in dopamine, inhibition of relaxation of the pelvic floor or inhibition of the pontine micturition centre [2], but methylphenidate is the drug of choice for resistant giggle incontinence. Commonly known as Ritalin, it is important in the treatment of attention deficit hyperactivity disorder (ADHD). Whilst it has been shown to have excellent success rates [2,7], it has an important side-effect profile which includes cardiac issues (hypertension, tachycardia) and psychological problems (mood change, aggression, suicidal ideation). It may also cause obscure complications – one patient of mine is an excellent dancer, and she developed a reversible foot drop. Treatment must be preceded with counselling, heart rate, blood pressure, weight and height measurement, assessment of appetite and psychiatric symptoms, and these must also occur following dose change and / or every six months of treatment. Chang reported 100% success rate of 12 months’ treatment but did not report long-term results [8].
The most interesting aspect of this study was the urodynamic changes before and after treatment. Apart from the observation that the few patients who had an overactive bladder pre-treatment became normoreflexic afterwards, none of the parameters showed any significant changes, except for maximum urethral closing pressure and maximum urethral pressure which showed significant increases. This is a target of interest which requires further study. Generally speaking, although results with methylphenidate have been reported as good after initial treatment, they may not be sustained, and the relapse rate is significant [3].
In summary, the diagnosis of giggle incontinence needs to be clear and not clouded by other types of voiding dysfunction. Conservative measures such as reassurance, timed voiding and biofeedback should be the first-line treatments [4,9] before considering pharmacological agents. Antimuscarinics are better tolerated and should be used as the first pharmacological agent, followed by methylphenidate in resistant cases.
References
1. Mackeith RC. Micturition induced by giggling? Archives of Disease in Childhood 1959;34(176):354-8.
2. Logan BL, Blais S. Giggle incontinence: Evolution of concept and treatment. Journal of Pediatric Urology 2017;13(5):430-5.
3. Hacıislamo glu A, Eks M, Noyan DO, et al. Evaluation of the efficacies of methylphenidate and biofeedback treatments in giggle incontinence: One-year follow-up study. Journal of Paediatric Urology 2021;17(5):646.
4. Richardson I, Palmer LS. Successful Treatment for Giggle Incontinence with Biofeedback. Journal of Urology 2009;182(4):2062-6.
5. Chandra M, Saharia R, Shi Q, Hill V. Giggle incontinence in children: a manifestation of detrusor instability. Journal of Urology 2002;168:2184-7.
6. Azim E, Mobbs D, Jo B, et al. Sex differences in brain activation elicited by humor. Proceedings of the National Academy of Sciences 2005;102(45):16496-501.
7. Berry AK, Zderic S, Carr M. Methylphenidate for giggle incontinence. Journal of Urology 2009;182(4 SUPPL.):2028-32.
8. Chang JH, Lee KY, Kim TB, et al. Clinical and urodynamic effect of methylphenidate for the treatment of giggle incontinence (enuresis risoria). Neurourology and Urodynamics 2011;30(7):1338-42.
9. Fernandes L, Martin D, Hum S. A case of the giggles Diagnosis and management of giggle incontinence. Canadian Family Physician 2018;64(6):445-7.
Declaration of competing interests: None declared.