Traumatic rupture of the tunica albuginea with either one or both corpora cavernosa of the penis is known as penile fracture. This may be associated with corpus spongiosum or urethral injury.
Incidence
Penile fracture was reported for the first time by Abul Kasem, an Arab physician, in Cordoba, Spain more than 1000 years ago [1]. It is not an uncommon condition but is often underreported [2]. It occurs more frequently in Middle Eastern and North African countries (almost 55% of the total number reported) than in the United States or Europe (almost 30% of those reported). Annual incidence in the USA is estimated at 500–600 cases, responsible for one in every 175,000 emergency admissions [3]. Concomitant urethral injury has been reported as high as 38% of cases, although the largest USA series suggests a lower rate of 23% [4].
Anatomy of penis
The penile shaft is made up of three erectile tissues: the two corpora cavernosa and a corpus spongiosum. Each corpora is covered by fascial layers containing nerves, lymphatics, and blood vessels. Externally, these are all covered by skin. Both corpora cavernosa are surrounded by the tunica albuginea, which displays outer longitudinal and the inner circular fibres. Proximally, at the base of the penis, these form the crura, which are attached to the ischiopubic rami. The tunica albuginea encasing the corpora cavernosa is 2mm thick when the penis is flaccid.
In the erect state, the tunica albuginea thins to 0.25–0.50mm and is thinnest ventrolaterally. During sexual intercourse, the intracorporeal pressure can reach 180mmHg, and the tunica albuginea can withstand values up to 1500mmHg. However, sudden flexion-based trauma to an already thinned tunica albuginea can result in rupture. Not unexpectedly, the most common site of rupture is ventrolateral at the thinnest aspect, often in the midshaft.
The urethra passes through the corpus spongiosum. This is very elastic relative to tunica albuginea, allowing expansion of the corpus spongiosum for passage of the ejaculate and urine through the urethra. Blood to the corpora cavernosa is supplied by paired deep arteries of the penis (cavernosal arteries), which run in the centre of each corpora cavernosa. All three cavernosa and spongiosa are surrounded by Bucks fascia, dartos fascia, and the penile skin.
Aetiology
Penile fractures are usually due to trauma during intercourse but can also occur secondary to non-sexual causes. They usually result from an abrupt blunt trauma by forceful bending of the erect penis. Typically it occurs during vigorous heterosexual coitus, whereby a failed attempt at vaginal insertion of the erect penis results in collision with the pubic bone or perineum. Sexual positions like the female partner on top or on all four limbs are associated with higher incidence. Other reported causes include vigorous intercourse, masturbation, falling off a bed, placing an erect penis in underwear and spontaneously fracturing the penis while urinating. In the Islamic world, instances of penile fracture may be accidentally self-inflicted by bending the erect penis to achieve rapid detumescence, known as taghaandan.
Injury can involve one or both of the corporal bodies and associated simultaneous urethral injuries may also occur. Penile fracture can be diagnosed clinically with history and physical examination. If there is doubt about the diagnosis adjuncts such as imaging may be used.
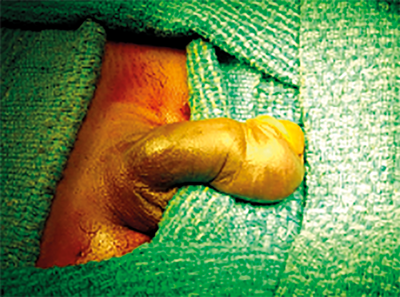
Figure 1. Aubergine sign.
Clinical features
Typically the history includes a sexual encounter involving trauma to the erect penis with an audible ‘pop’ or ‘cracking’ sound, pain, and rapid detumescence. The penis may become tense, swollen, and darkly discoloured (the ‘aubergine deformity’ – Figure 1) and penile deviation towards the side opposite to the injury. On palpation focal tenderness and a palpable defect in the tunica albuginea may help in diagnosing the fracture site. There is often a clot lying over or near the fracture site that corresponds to the site of cavernosal rupture (Figure 2).
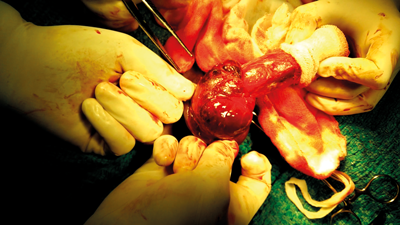
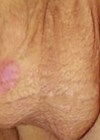
Figure 2. Subcutaneous haematoma.
Difficulty with urination or blood at the urethral meatus should raise suspicion of associated urethral trauma, although difficulty in voiding can also be secondary to compression of the urethra by haematoma. Urethral injury is observed in around one third of cases and is usually a partial disruption of urethra. Penile rupture can occur anywhere but is commonly localised at the base of the penis, just proximal to the penoscrotal junction. Often single corporal body is injured, but both corpora and the corpus spongiosum may be injured depending upon the severity of the injury.
A haematoma within the perineum, scrotum, or lower abdominal wall indicates rupture of Buck’s fascia: the extravasation of haematoma spreads along the Colles fascia and ecchymosis extends like a ‘butterfly’ over the perineum, scrotum, and lower abdomen. It is important to recognise that penile fracture can exist in the absence of classic findings and a high index of suspicion is required. The main differential diagnoses are ruptured superficial dorsal vein of penis or suspensory ligament injury.
Use of imaging in diagnosis of penile fracture
Penile fracture is predominately a clinical diagnosis, therefore imaging should not be routinely considered as it is likely to lead to unnecessary delays in diagnosis and increased morbidity [5]. This is particularly important out-of-hours as modern day radiology on-calls usually involve remote reporting or outsourcing to external companies so it is rare to find a radiologist on site overnight. There are rare cases in which imaging may be of benefit. Imaging should be considered in patients with a delayed presentation or if the history and examination are equivocal leading to an uncertain diagnosis.
The main aim of imaging is to confirm or exclude the presence of penile fracture. The location of the defect can be identified and thus the surgical incision can be made directly over the site of the defect to avoid the need for complete de-gloving of the penis [6].
Ultrasound should be the first-line investigation for penile fracture according to the current literature [7]. This is a fast, inexpensive and readily available test which in experienced hands can provide a definitive diagnosis of penile fracture. The penis is best imaged in long section. The tunica albuginea normally appears as a hyperechoic structure surrounding the hypoechoic corpus cavernosum and spongiosum. In the case of fracture there will be a hypoechoic break in the tunica albuginea, often with associated haematoma or oedema.
In reality it is often difficult to obtain images of diagnostic quality with ultrasound as pressure needs to be applied to the penis and this is not well tolerated due to pain. Also if there is a large haematoma present it can be difficult to view the tunica albuginea in its entirety making it difficult to confidently exclude fracture.
The quality of ultrasound is dependent on the skill of the operator. As penile fracture is an uncommon presentation there are very few sonographers or radiologists who have experience performing this examination, therefore you may encounter difficulties in finding an appropriately trained member of the radiology team to perform the scan.
MRI is becoming more widely used as it can demonstrate penile fractures in detail, identify urethral involvement, identify alternative diagnosis (such as suspensory ligament injury) and should be less painful for the patient. MRI is therefore the most accurate modality in the diagnosis or exclusion of penile fracture.
For the best quality diagnostic images a penile coil should be used with multi-planar T1, T2 and post contrast T1 images acquired [8]. In reality there are very few MRI departments who will have a specific penile coil as it is not a common examination.
In our unit, we use a pelvic / abdominal coil with the penis taped up to the lower abdomen. Small field of view sequences are then acquired with multi-planar T1, T2 and axial T1 post contrast (30s) images acquired.
The tunica albuginea is normally a low signal band on both T1 and T2. In the case of fracture there will be a high T2 signal defect in this band with surrounding oedema and haematoma.
The disadvantage of MRI is that it is costly, more time consuming than ultrasound and not routinely available out-of-hours. Therefore reliance on MRI to confirm a breach in the tunica may lead to delays in diagnosis.
Penile angiography has a role in the diagnosis and management of only a small minority of penile fractures. This is mainly used in cases of post-traumatic priapism to identify the source of bleeding and embolise the vessel responsible. It cannot identify the defect in the tunica albuginea. This is an invasive procedure and is only available at specialist centres with vascular interventional radiologists.
Historically the assessment of urethral involvement was done using retrograde urethrograms. This involves catheterising the terminal portion of the urethra and injecting contrast under fluoroscopic control. As you can imagine this is not well tolerated due to pain and can only identify urethral injury and not the defect in the tunica albuginea. This is no longer used in the acute phase but does still have a role postoperatively in assessing for strictures or fistulae [9].
Another historical imaging tool was cavernosography. This involves percutaneous injection of contrast into the corpus cavernosum under fluoroscopic guidance. This is an invasive procedure which requires an interventional radiologist to perform and was not well tolerated by patients due to pain. It is no longer routinely performed.
Management of penile fracture
Blunt trauma to the flaccid penis rarely results in significant injury and may only produce a subcutaneous haematoma. Usually no surgical intervention is needed and only analgesics and ice packs are required for treatment of these cases. In cases of penile fracture, emergency surgical exploration with closure of the tunica albuginea is the treatment of choice.
Early surgery (36 to 48 hours) [10] also results in significantly fewer complications vs. delayed surgery especially for penile curvature [11].
Conservative management
Conservative management is not advised for penile fracture as it is associated with poor long-term outcomes [12]. However, should a fully informed and competent patient adamantly refuse surgical intervention, they may be offered cold compressions and pharmacologic interventions to limit erections and advised to abstain from sexual activity for up to six weeks [11].
Non-surgical management predisposes the patient to the development of penile curvature, erectile dysfunction, and pain with intercourse in up to 60% of cases [13]. Additionally, failure to diagnose urethral injury may result in subsequent stricture or urethrocutaneous fistula.
Surgical management
Catheterisation
Urethral catheterisation should be done before surgery (if urethral injury has been excluded by history and examination or imaging). If there is clinical or radiological suspicion of a concurrent urethral injury, it is our practice to view the urethra directly with flexible cystoscopy. However, we are aware that some colleagues feel a cystoscopy is unnecessary as they will view the urethra directly when they deglove the penis and identify the corporal defect. If flexible cystoscopy is performed, pass a foley catheter urethrally following this. The catheter allows identification of the urethra and reduces the risk of inadvertent injury while dissecting the corporal bodies, as well as providing a scaffold for the repair of any associated urethral injury. The Foley catheter can be removed immediately after surgery unless a urethral injury was repaired, in which case it should be left in place for 10-14 days.
Choice of incision
Multiple incision sites have been proposed, including a circumcising degloving incision, midline penoscrotal, inguinoscrotal, and lateral incision. Each incision has its benefits but in most cases a degloving circumcising incision is recommended. This allows an evaluation of all three corporal bodies and the ability to repair injuries anywhere along the course of the shaft, as well as repair or separation of the neurovascular bundle and repair of the urethra if needed. However, this approach carries a risk of neurovascular insult with subsequent detriment to penile sensation and erectile function. In uncircumcised patients, historically circumcision was considered due to possibility of postoperative phimosis, however there is no conclusive data to support this practice in all patients.
A midline penoscrotal incision can be done if a degloving incision is difficult due to tissue oedema and haematoma or if the main haematoma / suspected site of injury is in the penoscrotal region. Additionally, this serves to avoid lymphoedema of the distal shaft skin, which can occur after degloving incisions and can be cosmetically unacceptable to some patients. Alternatively, a vertical or transverse incision can be made directly over the defect when the fracture is palpable or localised on imaging preoperatively.
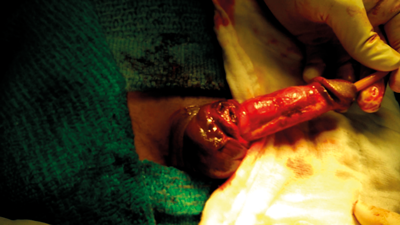
Figure 3. Degloving of penile shaft.
Technique
Adequate exposure and delineation of the site, size and any associated urethral / corpus spongiosum injury is essential. A single dose of antibiotics is given at induction.
During exploration the haematoma is evacuated with debridement of dead tissue and primary repair of the defect performed. Surgical exploration is traditionally done via a subcoronal circumferential incision (Figure 3), and penile skin degloved proximally up to the base. Usually the fracture site presents as a transverse laceration, between 0.5 and 2.0cm long, in the tunica albuginea (Figure 4). The edges of the opened tunica are only trimmed if deemed necessary. Absorbable sutures like polyglactin or polydioxanone 3-0 or 2-0 round body are used for closure of the tunica albuginea tear [11] (Figure 5). Corpus spongiosum injuries almost always occur at the same level as the corpora cavernosal injury. If the corpus spongiosum and urethra are injured, a two-layer closure is recommended with 4-0 synthetic absorbable suture. These type of injuries require a sub-dartos flap between the corpora cavernosa and corpus spongiosum, to prevent fistula formation. The Foley catheter should also be left indwelling for 10–14 days after surgery.
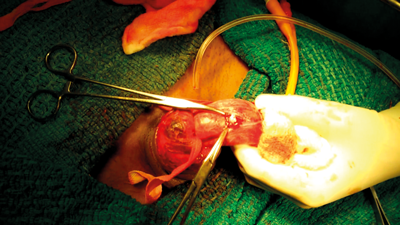
Figure 4. Site of rupture.
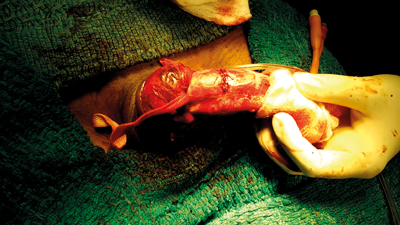
Figure 5. Repair of tunica albuginea defect.
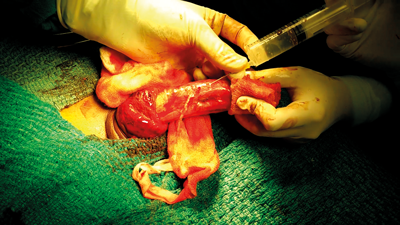
Figure 6. Saline injection in corpora cavernosa to confirm site of rupture.
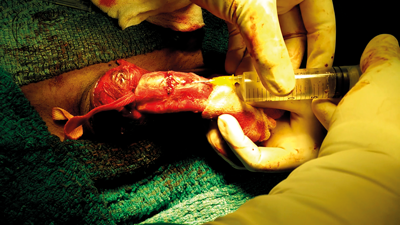
Figure 7. Saline injection to confirm adequacy of repair.
After surgical repair, penile tumescence should be induced to check the stability of the repair and for any missed corpora cavernosal injuries (Figure 6 shows a leak prior to repair, Figure 7 shows the same area after repair). This is done by placing a Penrose drain around the base of the penis with a clamp to act as a tourniquet. After the application of tourniquet, saline or saline mixed with indigo carmine is injected with a 22G needle in the corporal body on the lateral aspect. This creates tumescence and allows a clear evaluation of the repair and identification of any other corporal injuries. To exclude a corpus spongiosum injury, a 22G needle is placed in the glans penis and the corpus spongiosum is engorged with saline mixed with indigo carmine. This allows a visual inspection of the engorged corpus spongiosum and helps to identify any injury.
Postoperative management
Postoperatively anti-inflammatory agents are recommended for analgesia. Penile tumescence after surgery has been reported to cause dehiscence of the corporal repair .The decision to use anti androgen or sedatives is controversial as pain after surgery normally prevents fully rigid erections. Patients can be discharged after 24-48 hours of surgery and sexual activity can be restarted after six weeks [11]. In patients with urethral repair, a Foley catheter should be continued for two weeks following which a voiding cystourethrogram is done to confirm healing.
Postoperative complications
Postoperatively, superficial wound infection in 9% and erectile dysfunction in 1.3% have been reported [14]. Erectile dysfunction is usually self-limiting and resolves in three to four months.
Conclusion
Penile fracture is a urological emergency. It is usually a clinical diagnosis and although preoperative imaging is not mandatory, it can be used in equivocal clinical cases provided it does not delay surgical repair. Have a high index of suspicion for associated urethral injury and if suspected we would recommend flexible cystoscopy to assess the injury prior to definitive repair. Conservative management places the patient at increased risk for erectile dysfunction and penile curvature, whereas prompt surgical repair is associated with favourable long-term functional and cosmetic outcomes.
TAKE HOME MESSAGE
-
Surgeons should perform prompt surgical exploration and repair in patients with acute signs and symptoms of penile fracture.
-
Imaging may be used as an adjunct to clinical diagnosis provided this does not unduly delay surgery.
-
Clinicians may perform ultrasound in patients with equivocal signs and symptoms of penile fracture.
-
MRI could be considered as an alternative to ultrasound or in cases when ultrasound is equivocal.
-
If imaging is equivocal or diagnosis remains in doubt, surgical exploration should be performed.
-
Clinicians must perform evaluation for concomitant urethral injury in patients with penile fracture or penetrating trauma who present with blood at the urethral meatus, gross haematuria or inability to void.
References
1. Taha SA, Sharayah A, Kamal BA, et al. Fracture of the penis: surgical management. Int Surg 1988;73:63-4.
2. Eke N. Fracture of the penis. Br J Surg 2002;89:555-65.
3. Pariser JJ, Pearce SM, Patel SG, et al. National patterns of urethral evaluation and risk factors for urethral injury in patients with penile fracture. Urology 2015;86(1):181-5.
4. Amit A, Arun K, Bharat B, et al. Penile fracture and associated urethral injury: experience at a tertiary care hospital. Can Urol Assoc J 2013;7(3-4):168-70.
5. Masarani M, Dinneen M. Penile fracture: diagnosis and management. Trends in Urology Gyneacology & Sexual Health 2007;Sep/Oct:20-22.
6. Harbiyeli M, Abol-Enein H, Johansen TEB. Diagnosis and treatment of penile fractures: a single centre series. Open Journal of Urology 2017;7:31-9.
7. Nicola R, Carson N, Dogra VS. Imaging of traumatic injuries to the scrotum and penis. American Journal of Roentgenology 2014;202(6):512-20.
8. Choi MH, Kim B, Ryu JA, et al. Imaging of acute penile fracture. Radiographics 2000;20:1397-405.
9. Pompili G, Munari A, Campari A, et al. Traumatic penile fracture: what radiologist should know. European Society of Radiology 2014; Poster C-0695.
10. De Luca F, Garaffa G, Falcone M, et al. Functional outcomes following immediate repair of penile fracture: a tertiary referral centre experience with 76 consecutive patients. Scand J Urol 2017;51:170-5.
11. Vilson F, Macdonald S, Terlecki R. Contemporary management of penile fracture: a urologist’s guide. Curr Sex Health Rep 2016;8(2):91-6.
12. Swanson DE, Polackwich AS, Helfand BT, et al. Penile fracture: outcomes of early surgical intervention. Urology 2014;84(5):1117-21.
13. Ozorak A, Hoscan MB, Oksay T, et al. Management and outcomes of penile fracture: 10 years’ experience from a tertiary care center. Int Urol Nephrol 2014;46(3):519-22.
14. Orvis BR, McAninch JW. Penile rupture. Urol Clin North Am 1989;16:369.
Declaration of competing interests: None declared.