Case 1
A 26-year-old male presented with a two-week history of testicular pain and swelling. On examination the right testicle was enlarged, indurated and tender. Erythema of the scrotum on that side was also noted. Ultrasound of the testis reported a distorted right testicle with irregular solid and cystic components suggestive of a focal abscess with an inflammatory mass (Figure 1). Doppler study confirmed absence of any obvious internal vascular signal but with an increase in the peripheral vasculature (Figure 2).
This was diagnosed as epididymo-orchitis with intratesticular abscess formation and managed accordingly. However, a repeat ultrasound scan five weeks later demonstrated no resolution of the presumed inflammatory mass. The appearances were now more in keeping with malignancy and his serum lactate dehydrogenase (LDH) levels were found to be elevated. Other tumour markers (β-HCG and AFP) were within normal limits. He underwent a radical inguinal orchidectomy. Histology confirmed a mixed germ cell tumour.
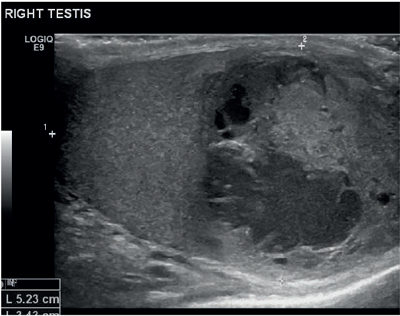
Figure 1.
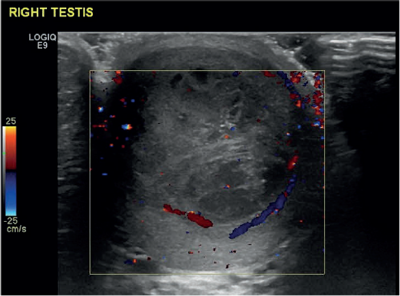
Figure 2.
- What proportion of testicular malignancies present with pain?
- List three other atypical presentations that clinicians should be aware of in the diagnosis of testicular cancer.
Case 2
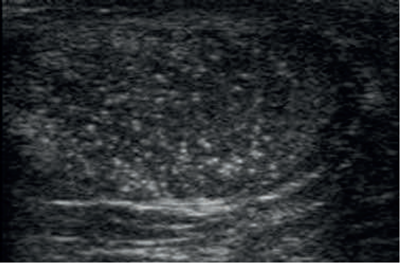
- What is the diagnosis from this ultrasound scan?
- What is the prevalence of this condition in the asymptomatic general population and the incidence of malignancy?
- What is the prevalence of this condition in the sub-fertile population and the incidence of malignancy in this sub-population?
- What are the criteria you would use to select the men who require further investigation and treatment for this condition? What is the rationale for doing this?
Case 3

This photograph represents a retroperitoneal lymph node dissection (RPLND) for advanced germ cell tumours of the testis.
- What is the likely pathology of residual tumour after chemotherapy for non-seminoma, with likely incidences?
- What further treatment are required if mature teratoma and the fibrotic mass is completely removed?
- What are the recommended management options for residual mass of seminoma?
Testicular cancer – answers
Case 1
-
Up to 20% of patients may present with testicular pain within the mass, usually due to haemorrhage or infarction of the tumour [1].
-
Patients with testicular cancer may present in the following atypical ways [1]:
-
With a hydrocele.
-
Gynaecomastia or nipple tenderness if beta human chorionic gonadotrophin (hCG) levels are elevated, and in men with Leydig cell tumours.
-
Weight loss, palpable abdominal or neck mass, flank or back pain, or pulmonary, neurological or gastrointestinal complaints when patients present with advanced disease.
Case 2
-
Testicular microlithiasis.
-
Testicular microlithiasis has a prevalence of about 5% in the general population. The incidence of testicular malignancy as a percentage of men with microlithiasis is 1% [2,3].
-
The prevalence of testicular microlithiasis in the sub-fertile population is 2.4%, and in this population men with testicular microlithiasis have a 4% incidence of testicular cancer [3].
-
Men who can be qualified by what is known as the testicular dysgenesis syndrome (TDS) should be considered for further investigation and treatment. These include men presenting with sub-fertility, history of cryptorchidism, testicular atrophy and unilateral testicular germ cell tumour (TGCT). Testicular microlithiasis has not been associated with an increased prevalence of intratubular germ cell neoplasia (ITGCN) in healthy asymptomatic men, but in those with the risk factors listed above. ITGCN is a premalignant lesion and is known to lead to TGCT [2,3,4].
Case 3
-
Following first-line bleomycin, etoposide, cisplatin (BEP) chemotherapy the pathology of residual tumour is found to have 6-10% viable cancer, 50% contain mature teratoma and 40% contain necrosis and fibrosis [5,6].
-
No further treatment is required.
-
A residual mass of seminoma should not be primarily resected as residual masses from seminoma tend to be intensely fibrotic and difficult to remove, although RPLND may be possible in certain centres of excellence when indicated [5]. FDG-PET scans, tumour markers and biopsies help ascertain the extent and nature of the retroperitoneal mass. Salvage therapy in the form of chemotherapy or radiotherapy are the usual options.
References
1. Stevenson SM, Lowrance WT. Epidemiology and diagnosis of testis cancer. Urol Clin N Am 2015;42:269-75.
2. Sharma P, Dhillon J, Sexton WJ. Intratubular germ cell neoplasia of the testis, bilateral testicular cancer, and aberrant histologies. Urol Clin N Am 2015;42:277-85.
3. van Casteren NJ, Looijenga LH, Dohle GR. Testicular microlithiasis and carcinoma in situ overview and proposed clinical guideline. Int J Androl 2009;32(4):279-87.
4. Tan IB, Ang KK, et al. Testicular microlithiasis predicts concurrent testicular germ cell tumours and intratubular germ cell neoplasia of unclassified type in adults. A meta-analysis and review. Cancer 2010;116:4520-32.
5. Albers P, Albrecht W, Algaba F, et al. Guidelines on Testicular Cancer. European Association of Urology; 2015. Accessed from www.uroweb.org.
6. Heidenreich A, Thuer D, Polyakov S. Postchemotherapy Retroperitoneal Lymph Node Dissection in Advanced Germ Cell Tumours of the Testis. European Urology 2008;53:260-74.





