- Click for Part 1 and Part 3 on this topic -
Case scenario
A 37-year-old male presents to A&E with 12 hours of intermittent, severe, left-sided loin to groin pain and multiple episodes of vomiting. Urine dipstick shows 2+ blood but no other abnormalities. He undergoes imaging as part of his investigations.

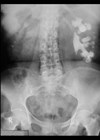
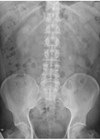
Figure 1.
1a) Describe Figure 1 and the acute urological diagnosis.
On review the patient is clinically well with no fever and normal renal function. His pain is well controlled using oral analgesia. You decide to pursue active primary treatment.
1b) What management options are available for this patient?

Figure 2.
2a) What is shown in Figure 2?
2b) How does extracorporeal shockwave lithotripsy (ESWL) work in the treatment of urinary tract calculi?
2c) What factors are associated with treatment success?
2d) What are the contraindications to ESWL? The patient undergoes two sessions of ESWL with successful stone fragmentation. He presents to A&E three weeks later with worsening left flank pain. A repeat CT of kidney, ureters and bladder (KUB) is conducted.

Figure 3.
3. Describe the complication demonstrated in Figure 3.
Answers
1a) This is a coronal reconstruction of an unenhanced low dose CT KUB in the soft tissue window which demonstrates a 9mm (craniocaudal length) left upper ureteric calculus with associated periureteric fat stranding and dilatation of the partially visualised renal pelvis.
1b) Primary ureteroscopy (URS) and stone extraction +/- laser stone fragmentation. Extracorporeal shockwave lithotripsy (ESWL) – if available in a timely fashion, this management option offers a successful non-invasive treatment option, with high patient tolerability, that can be delivered in an outpatient setting under local anaesthetic [1].
The Getting it Right First Time (GIRFT) acute stone pathway recommends definitive stone treatment for patients requiring intervention within 48 hours [2]. This could be either primary URS or ESWL.
European Association of Urology (EAU) guidelines for management of ureteric calculi [3]: for definitive management of ureteric stones <10mm equal weight is given to SWL or URS regardless of location.
2a) Figure 2 shows fluoroscopic targeting of the ureteric stone during ESWL (obtained using Storz Modulith SLX-F2).
2b) A pulsewave or high energy acoustic shockwave is generated outside the body using either electrohydraulic, electromagnetic or piezoelectric methods. The acoustic energy wave generated is transferred through the soft tissue of the body, targeting the calculus. Calculus localisation in the ureter is performed using X-ray and precise localisation reduces surrounding tissue damage.
There are numerous mechanisms describing how pulsewaves may fragment stones and whilst not fully understood, the following two resulting mechanical forces are thought to be most relevant:
- Direct stress associated with the high amplitude shockwave resulting in stone fragmentation.
- Mechanical stresses associated with the growth and collapse of cavitation bubbles within the stone [4].
The frequency (rate) and intensity (energy) of the pulsewave can be modified by the operator during the procedure to optimise stone fragmentation. A slower pulse rate has been shown to be more effective for stone fragmentation, potentially by allowing cavitation to work more efficiently [4].
2c) The main negative factors associated with ESWL success are proximally located stones, larger stones, skin to stone distance >10cm and higher stone density. Stones with <970HU on CT were significantly more likely to be successfully treated with ESWL (98% vs. 38%) [5]. The presence of hydronephrosis may also reduce the efficacy of ESWL [6].
2d) Absolute contraindications [7]:
- Pregnancy
- Uncorrected coagulopathy or bleeding diathesis
- Aortic aneurysm (particularly with calcified walls)
- Severe untreated hypertension
- Untreated urinary tract infection.
3. Figure 3 is a sagittal reconstruction of a CT KUB in the bone window demonstrating a column of small stone fragments within the left lower ureter extending 3cm in length, with mild upstream hydroureter in keeping with steinstrasse.
Steinstrasse, the German word for ‘Stone street’, describes a possible complication of ESWL where a column of stone fragments cause obstruction. The most common site for this fragment column is the distal ureter (64% of cases). The incidence of steinstrasse has greatly decreased from 20% to 6% due to a refinement in ESWL technique [8]. Management options for steinstrasse are similar to that of a primary obstructing calculus.
References
1. Güler Y. Non-contrast computed tomography-based factors in predicting ESWL success: A systematic review and meta-analysis. Progrès en Urologie 2023;33(1):27–47.
2. https://gettingitrightfirsttime.co.uk/
wp-content/uploads/2021/12/Urology
_2021-12-10_Guidance_Acute-stones.pdf
[accessed 22 January 2026].
3. https://uroweb.org/guidelines/urolithiasis
[accessed 22 January 2026].
4. Cleveland R, McAteer J. Physics of Shockwave Lithotripsy. In: Smith AD, Badlani GH, Preminger GM, Kavoussi LR (Eds.). Smith’s Textbook of Endourology, 3rd Edition Wiley Blackwell; 2012:317–32.
5. Ouzaid I, Al-qahtani S, Dominique S, et al. 2012. A 970 Hounsfield units (HU) threshold of kidney stone density on non-contrast computed tomography (NCCT) improves patients’ selection for extracorporeal shockwave lithotripsy (ESWL): evidence from a prospective study. BJU Int 2012;110(11 Pt B):E438–42.
6. Chang KD, Lee JY, Park SY, et al. Impact of pretreatment hydronephrosis on the success rate of shock wave lithotripsy in patients with ureteral stone. Yonsei Med J 2017;58(5):1000–5.
7. Reynolds LF, Kroczak T, Pace KT. Indications and contraindications for shock wave lithotripsy and how to improve outcomes. Asian J Urol 2018;5(4):256–63.
8. Sayed MA, el-Taher AM, Aboul-Ella HA, Shaker SE. Steinstrasse after extracorporeal shockwave lithotripsy: aetiology, prevention and management. BJU Int 2001;88(7):675–8.